Minnies finalists, page 2
Best Radiologist Training Program
Emory University Hospital, Atlanta, GA

The finalists for Best Radiologist Training Program this year include a frequent Minnies' nominee across a variety of categories, Emory University Hospital in Atlanta, and a newcomer to the nomination, the University of Mississippi in Jackson. Emory won the category in 2021.
Emory can trace its radiology lineage back to the 1940s when it established a department of radiology under the leadership of Heinz Stephen Weens, MD. In 2011, what was then called the Department of Radiology became the Department of Radiology and Imaging Sciences to encompass a broader arena of clinical specialization and scientific advances.
The university's training program features a four-year diagnostic radiology residency. The residency's program director is led by Ryan Peterson, MD, a neuroradiologist whose clinical interests include neurotrauma and general neuroradiology. The university also offers an interventional radiology residency that trains participants in interventional oncology and transplant and reproductive health interventions. Finally, through its School of Radiologic Technology, Emory offers a 24-month certification program that incorporates both classroom and clinical instruction.
Emory takes pride in being one of the largest academic radiology practices in the U.S. Through its diagnostic radiology residency, it provides training in the form of specialized tracks, including a Clinical Educator track for academic radiology careers; a Global Health track that "develops residents' expertise in topics of public health and policy, their understanding of the challenges involved in improving access to radiology services in resource-limited settings, and their cultural competency"; an Integrated Imaging Informatics track; a Molecular Imaging in Medicine track; a Quality Improvement and Innovations track; and a Research track.
"Personalization of radiology education is what sets us apart," said Peterson.
University of Mississippi Medical Center, Jackson, MS

The University of Mississippi Medical Center in Jackson is the only academic center in the state, as well as the only organ transplant center, the only level I trauma center, and the only children's hospital, according to diagnostic radiology residency program director Charlotte Taylor, MD. The department's chair is Rich Duszak, MD.
"Our catchment is the entire state, and we serve the sickest patients, so our residents are exposed to complex cases," Taylor said.
As part of the diagnostic radiology residency, the university's radiology department offers a number of tracks, including an Early Specialization in Interventional Radiology (ESIR) track, a combined radiology residency/PhD track, and a molecular imaging track; a clinical educator track is in the works. Residents also benefit from the department's contrast reaction simulation laboratory.
"Our training environment well-prepares our graduating residents and fellows for any academic or private practice environment," Taylor said.
Best Radiologic Sciences Program
This year’s Minnies finalists for the Best Radiologic Sciences Training Program include a four-time winner and a university seeking its first Minnie in this category.
Thomas Jefferson University, Philadelphia, PA

Nestled in one of the most populous U.S. cities, Thomas Jefferson University (TJU) is no stranger to the Minnies. The university won the award for Best Radiologic Sciences Training Program in 2014, 2017, 2019, and 2022.
The Department of Medical Imaging and Radiation Sciences at TJU was built with the mission of education and opportunity. It has graduated students for over 35 years with a bachelor’s degree and dual concentrations in the medical imaging profession.
Students have the opportunity to gain the knowledge, skills, and behaviors to work in two different medical imaging and radiation sciences concentrations. These include radiography, MRI, CT, invasive cardiovascular technology, radiation therapy, medical dosimetry, abdomen-extended and ob/gyn sonography, vascular sonography, and cardiac sonography.
“Our students and graduates are the success of our programs," said department chair Colleen Dempsey, herself a Minnies finalist for Most Effective Radiologic Sciences Educator. "They are well-rounded, professional, caring, and competent medical imaging and radiation sciences professionals. They are highly sought out by employers and become leaders in our profession. “This is a testament to our dedicated and expert faculty who live our Department mission to provide a comprehensive education preparing students for entry-level practice in medical imaging and radiation sciences as competent, caring members of the healthcare team, cultivating professionalism and life-long learning.”
Dempsey added that students get hands-on learning experiences that incorporate classroom, clinical, and lab education.
Some of the lab equipment includes the following: a virtual environment radiotherapy training (VERT) room, a dosimetry lab with three planning systems, a laser patient positioning radiation therapy lab, phantom models for students to train on, radiation therapy immobilization device fabrication labs and equipment, and mobile x-ray machines among others.
Quinnipiac University, Hamden, CT

Quinnipiac University and its educators have been named as semifinalists in the Minnies in previous years, but the institution, located in Hamden --"The Land of the Sleeping Giant," -- is still seeking its first award in all categories.
Quinnipiac’s radiologic science program is a three-year accelerated bachelor’s degree program that also offers an optional “3+1” program. The latter refers to three years of study in the bachelor’s in radiologic sciences program (undergraduate) plus an optional additional year of study in the university’s Master of Health Science in advanced medical imaging and leadership (graduate). This means graduates earn a bachelor's and a master's degree in four years.
“Our on-campus lab space is incredible,” said Kori Stewart, PhD, director of Quinnipiac’s radiologic sciences program. “We have two energized digital x-ray rooms and a portable unit which are in the diagnostic imaging department’s imaging suite. This imaging suite also includes CT, MRI, mammography, bone densitometry, and sonography."
Students also have opportunities to get involved in nontraditional imaging, both as it relates to research and forensic imaging. They participate in imaging at the Office of the Chief Medical Examiner in Farmington, CT, in their senior year of the undergraduate portion of their degree.
The university’s radiologic sciences program has “exceptional” outcomes with a five-year American Registry of Radiologic Technologists (ARRT) pass rate above the national average.
“Our graduates go on to become leaders in the field of radiologic sciences and diagnostic imaging,” Stewart said.
Will this be Quinnipiac’s year to finally capture that elusive first Minnie, or will TJU remind everyone again why it's had so many accolades?
Most Significant News Event in Radiology
CMS backs reimbursement for CT colonography
In July, the U.S. Centers for Medicare and Medicaid Services (CMS) indicated that it would advocate for Medicare reimbursement for CT colonography for colorectal cancer screening, including it in its proposed 2025 Hospital Outpatient Prospective Payment System (HOPPS) and 2025 Medicare Physician Fee Schedule (MPFS) rules. The American College of Radiology (ACR) -- which has been urging this coverage since 2008 -- praised the CMS' position change, noting that it is "a big step forward toward providing Medicare patients access to a minimally invasive colorectal cancer screening tool that can detect precancerous polyps and does not require anesthesia." The American Cancer Society, the U.S. Preventive Services Task Force, and the U.S. Food and Drug Administration (FDA) support Medicare coverage of the exam, but the CMS has denied it for years and has continued to take that position.
Covering the screening exam is crucial for keeping American men healthy, since colorectal cancer is the leading cause of cancer death in men under 50 in the U.S., advocates for reimbursement have noted. As well, the disease affects Black men more than their white or Hispanic counterparts: This population is 20% more likely to get colorectal cancer and 40% more likely to die from it.
In its announcement that it would back Medicare coverage of CTC, the CMS wrote that CTC is a "reasonable and necessary … colorectal cancer screening test, especially for patients and clinicians who seek a direct visualization procedure as a first step in CRC screening that is less invasive and less burdensome on the patient and healthcare system compared with screening colonoscopy," but it also urged clinicians to educate patients on the risks of the exam when it comes to radiation exposure and potential follow-up of incidental findings.
Medicare coverage would certainly give a boost to the utilization of CTC. One study suggested that reimbursement for CTC could not only increase uptake of the exam but also mitigate colorectal cancer screening disparities, particularly racial and socioeconomic ones; another study found that colon cancer screening reduces mortality rates at 10-year follow-up -- results that underscore the promise CTC shows for screening for the disease.
Will Medicare coverage for CTC be included in the CMS' final rules, which tend to be released late in the year? Keep an eye out for AuntMinnie.com's coverage to find out.
Researchers explore radiology applications for large language models
The second nomination for the category regards the exploration of radiology applications for large language models (LLMs). The topic has prompted a plethora of studies, from research that suggested that LLMs can not only simplify radiology reports but that they can also generate summaries that would help patients better understand these reports. Two works published this year found that direct radiologic image inputs can improve the diagnostic accuracy of LLMs and that an open-source LLM (Meta's Llama 3 70B) offers comparable performance to proprietary models when it comes to multiple-choice radiology test questions.
Researchers from the University of Maryland reported that smaller, "fine-tuned" LLMs for imaging applications are more sustainable than large general-purpose ones, since they use less energy without negatively affecting accuracy. And most recently at the Society for Imaging Informatics in Medicine's (SIIM) Conference on Machine Intelligence in Medical Imaging (CMIMI), Eliot Siegel, MD, of the University of Maryland in Baltimore offered an overview on advances in LLMs that may translate to not only improved operations in the radiology department but better patient care.
In any case, the role LLMs will play in the imaging sphere continues to develop, and AuntMinnie.com will continue to provide up-to-date analysis.
Biggest Threat to Radiology
Private equity/corporatization of radiology
Is the growing influence of private equity in radiology a good thing or a bad thing? It depends on who you ask.
Supporters hail the benefits of outside investment for increasing the financial stability of radiology practices and supporting investments in new equipment and technologies. Meanwhile, critics point to the focus on short-term profits that increase radiologist workload and the risk of radiologists becoming commoditized workers as well as losing their leverage and negotiating power.
One thing’s for sure. With private equity/corporatization of radiology being voted by our expert panel as one of the two biggest threats to radiology, this market dynamic remains highly controversial.
Workforce shortages
Workforce shortages have been a real challenge in radiology over the last few years. There are simply not enough radiologists.
And it’s not just radiologists. In a recent survey, the American Society of Radiologic Technologists reported an 18.1% vacancy rate for radiologic technologists, up from 6.2% in 2021.
Although some ideas have been proposed to alleviate the shortages of radiologists and technologists, it’s clear that this problem won’t be going away any time soon.
Hottest Clinical Procedure
Photon-counting CT
This is photon-counting CT’s fourth straight year as a finalist for the Hottest Clinical Procedure (it was edged out in the final last year by the use of AI predictions).
Photon-counting CT (PCCT) directly captures x-ray photons as electric signals without having to then convert them to light, as conventional CT has to do. This capability translates to better spatial resolution, higher iodine image contrast, and better radiation dose efficiency, studies suggest.
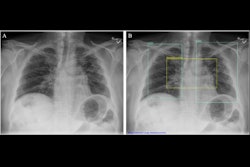
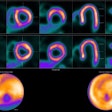
 Axial contrast-unenhanced abdominal CT examinations in a 38-year-old female patient with a body mass index (calculated as weight in kilograms divided by height in meters squared) of 31.23 with known renal calculi for recurring events of flank pain. The patient underwent (A) dose-optimized energy-integrating detector CT (1.49 mSv) and (B) submillisievert photon-counting detector CT (0.94 mSv). Images from both examinations showed a 3-mm calculus in the left kidney (arrows). Image and caption courtesy of the RSNA.
Axial contrast-unenhanced abdominal CT examinations in a 38-year-old female patient with a body mass index (calculated as weight in kilograms divided by height in meters squared) of 31.23 with known renal calculi for recurring events of flank pain. The patient underwent (A) dose-optimized energy-integrating detector CT (1.49 mSv) and (B) submillisievert photon-counting detector CT (0.94 mSv). Images from both examinations showed a 3-mm calculus in the left kidney (arrows). Image and caption courtesy of the RSNA.
At this year’s Society for Cardiovascular Computed Tomography annual meeting in Washington, DC, for instance, one presentation suggested that PCCT has the potential to revolutionize cardiac imaging. In addition, studies published a few weeks apart in Radiology in September suggest that PCCT can reduce radiation doses in lung transplant patients and serve as an alternative for assessing fatty liver disease.
As more of the systems are installed across radiology departments, PCCT may indeed live up to its promise as "the first new quantum leap in CT technology in a decade."
Theranostics

Theranostics has picked up so much momentum that it is driving the equivalent of an “industrial revolution” in nuclear medicine, according to experts.
Theranostics is a portmanteau of "therapy" and diagnostics" and refers to the dual approach of using the same molecular ligands to both image and treat cancer. It is a relatively simple concept that can be summed up with the expression, “See what you treat and treat what you see.”
While one could argue that the approach isn’t “new” (nuclear medicine departments have provided thyroid cancer treatment with a pair of radioactive iodine radioisotopes since the first half of the 20th century), the technique found new legs with the development of prostate-specific membrane antigen (PSMA) imaging agents and the approval of lutetium-177 PSMA-617 (Pluvicto, Novartis) for treating men with prostate cancer in March 2022.
Today, the approach is also being used successfully to treat neuroendocrine tumor patients and initial studies show encouraging results in patients with treatment-refractory meningioma. Moreover, the development and production of new radioisotope imaging and therapeutic agents is proceeding at full steam.
Will the first time in the finals be the ticket for theranostics? Stay tuned to find out.