Elevated liver fat fraction (LFF) identified on coronary CT angiography (CCTA) imaging appears to be an independent prognostic factor for major adverse cardiovascular events (MACE) in patients with type 2 diabetes, researchers have reported.
The findings could help better prevent MACE in these individuals, wrote a group led by Min Wang, PhD, of Shengjing Hospital of China Medical University in China. The team's results were published April 2 in Cardiovascular Diabetology.
"[Our study found that] incorporating LFF with [patients'] Framingham Risk and coronary artery calcium scores provided incremental predictive power for MACE in patients with type 2 diabetes," the group noted.
Type 2 diabetes is associated with higher risk of MACE, highlighting the need for accurate risk prediction, Wang and colleagues explained. Coronary artery calcium scoring (CACS) is an established tool for MACE risk assessment, but it may not capture all risk factors. Since hepatic steatosis is a common comorbidity in patients with diabetes, measuring it could help clinicians more thoroughly assess MACE risk level.
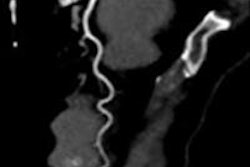
The team conducted a study that included 265 type 2 diabetes patients who presented at Shengjing Hospital with symptoms of chest distress and pain suggesting coronary artery disease between August 2021 and August 2022. All patients underwent both CCTA and upper abdominal dual-layer spectral detector CT (SDCT) exams within a seven-day period. The researchers tracked study participants' clinical data, CCTA imaging features, and liver fat fraction as determined by spectral detector CT. Among the patient cohort, 51 cases of MACE were documented over a median follow-up of 30 months.
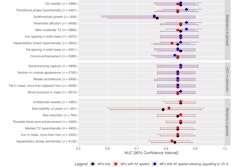
The investigators found that, compared with the traditional Framingham Risk Score model alone, the model that included liver fat fraction, CACS, and Framingham Risk Score information showed "stable clinical net benefit and demonstrated better predictive performance." They also found the following:
- The liver fat fraction in type 2 diabetes patients who experienced MACE was significantly higher compared with those who did not (p < 0.001).
- Patients with higher liver fat fraction were more likely to develop MACE, regardless of Framingham Risk or CAC score.
- Even after adjusting for early revascularization, both liver fat fraction and CACS were independently associated with MACE.
The takeaway? Incorporating liver fat fraction information with patients' Framingham Risk and CAC scores offers an additional way to stratify MACE risk in diabetic patients, according to the authors.
"[Our] study findings may guide personalized prevention for type 2 diabetes patients at higher MACE risk," they concluded.
The complete research can be found here.