For young women with a high genetic risk of breast cancer, twice-yearly MRI exams are more effective for detecting early disease than an annual mammogram, according to new research presented at the 2017 San Antonio Breast Cancer Symposium (SABCS).
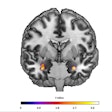
Researchers from the University of Chicago and the University of Washington in Seattle found that an intensive surveillance protocol consisting of a dynamic contrast-enhanced MRI exam (DCE-MRI) every six months was much more effective than an annual mammogram in detecting breast cancer in younger women with a high-risk genetic profile.
"This study demonstrates, for the first time, that aggressive breast cancers can be caught early, without excessive recalls or biopsies," said Dr. Olufunmilayo Olopade, director of the University of Chicago Center for Clinical Cancer Genetics, in a statement released by the university. "Because of intensive surveillance and high-quality care, the majority of high-risk women in this study -- most of whom had highly penetrant genetic mutations -- have not developed breast cancer."
Highest risk
The group's research goal was to understand the screening needs of women with the highest risk for breast cancer, said study co-author Mary Claire King, PhD, of the University of Washington, in the statement.
"Women with mutations in BRCA1 or BRCA2 have very different needs for surveillance for breast disease than do women with no mutations in these genes," she said. "This is particularly true for healthy young women with mutations."
The study included 305 women with a lifetime breast cancer risk greater than 20%. Of these, more than half (53%) had mutations in breast cancer-related genes, such as BRCA1, BRCA2, or CDH1. The women also had mutations in one of 11 known breast cancer-related genes, a diagnosis of breast cancer or carcinoma in situ before age 35, or a mother or sister diagnosed with breast cancer before age 50 (before age 40 for those with African ancestry).
Study participants underwent clinical breast examination and a DCE-MRI exam every six months and a digital mammogram every 12 months. They also had a BROCA panel (a breast cancer gene mutation test developed by the University of Washington) performed to identify any of 12 genes associated with a predisposition to breast cancer. Those with high genetic risk mutations who completed five years of follow-up were offered continued screening, according to Olopade's team.
Over the study time frame, each participant underwent about seven DCE-MRI scans (for a study total of 2,111) and four mammograms (for a study total of 1,223). Seventeen cancers were identified: four were ductal carcinoma in situ (DCIS), and 13 were early-stage breast cancer. Fifteen of these 17 cancers were found in participants with pathogenic mutations, while 11 involved BRCA1, three involved BRCA2, and one involved CDH1.
None of the cancers had spread to the lymph nodes, and all cancers detected during the study were smaller than 1 cm (mean tumor size was 0.61 cm), Olopade and colleagues reported.
The 17 patients who developed a cancer were followed continuously for a median of 5.3 years. All remain alive and free of systemic disease, according to the team.
"Mammograms remain important for most women," Olopade said. "But for women at high risk who are getting a DCE-MRI every six months, annual mammograms could probably be eliminated. For this group of younger women at significantly elevated risk, especially those with a BRCA1 mutation, we strongly support getting a DCE-MRI every six months."




.fFmgij6Hin.png?auto=compress%2Cformat&fit=crop&h=100&q=70&w=100)




.fFmgij6Hin.png?auto=compress%2Cformat&fit=crop&h=167&q=70&w=250)