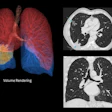
A Japanese study has found that high-resolution CT analysis can be used to successfully manage small solitary pulmonary nodules (SPNs). The practice could potentially obviate the need for some follow-up exams and biopsies.
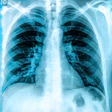
Most SPNs detected on chest radiographs are benign; however, primary lung cancer has been found in up to 38% of patients who underwent surgery for small SPNs detected in CT, wrote Dr. Shodayu Takashima and colleagues from Shinshu University of Matsumoto and Azumi General Hospital of Nagano, Japan.
And while previous studies have successfully used nodule characteristics as a basis for patient management, limited resolution has hindered the examination of nodules 1 cm and smaller, resulting in a substantial follow-up burden, they wrote (American Journal of Roentgenology, April 2003, Vol. 180:4, pp. 955-964).
"Until now, two-year (nodule) stability and benign calcification on radiography or CT have been used for predicting benign nodules," Takashima and colleagues wrote. "However, the observation policy will burden patients with additional costs, and the accuracy of invasive diagnostic procedures such as CT-guided biopsy is significantly (lower) for small lung nodules than for larger nodules."
Thus, the aim of the study was to establish reliable CT features for benign lesions in small pulmonary nodules, as defined as those 1 cm and smaller, in an effort to reduce the burden of follow-up. One can also envision the beneficial use of nodule features in computer-aided detection schemes.
Radiologists examined 13,786 subjects age 40 and older (54% men, 46% women; 54% smokers, 46% nonsmokers) using a low-dose chest CT protocol on a CT-W950SR scanner (Hitachi Medical Systems, Tokyo). Nine percent of the subjects were scanned again to follow up suspicious findings, and 26% were screened three times over the course of the study.
Two radiologists working independently read all of the images on a monitor, reviewing prior studies side by side. They made qualitative assessments as to the presence or absence of lobulation, spiculation, air bronchogram, cavity, satellite lesions, pleural tag, concave margins, and polygonal shape. They also performed quantitative evaluations of lesion size as a percentage of ground-glass opacity areas, and 2D and 3D ratios of lesions.
Lung cancer was diagnosed in 73 patients, including 61 cases of adenocarcinoma (31%), eight of squamous cell carcinoma, and four of small cell carcinoma. Atypical adenomatous hyperplasia was found in nine patients, and benign lesions in 53. Ten patients were lost or refused follow-up.
After excluding patients lost to follow-up or those with lesions thought to be benign, 135 cases remained, 72 of which were SPNs 1 cm or smaller. These cases were the focus of the retrospective arm of the study, which sought to predict cancers among small, indeterminate SPNs with the aim of reducing follow-up.
Based on surgical and histological results, the 72 cases yielded 25 lung cancers (35%), seven atypical adenomatous hyperplasias (10%), and 40 benign lesions, none in patients known to have extrapulmonary malignancies. Nineteen (76%) of the 25 lung cancers were localized bronchioalveolar carcinoma, five (20%) were adenocarcinoma with bronchioalveolar carcinoma components, and one (4%) was squamous cell carcinoma, the authors wrote.
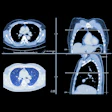
All 72 patients underwent diagnostic CT twice: first conventional CT scans with contiguous 10-mm sections, then spiral CT through the lesions with sequential 1-mm sections during a breath-hold, reconstructed at 0.5-mm intervals using a bone algorithm. Next, three to five coronal multiplanar reformations were acquired at 1-mm intervals.
The two readers independently estimated the likelihood of each lesion being benign or malignant using a 100-point scale based on a qualitative assessment of the high-resolution CT images. Lesions scoring under 50 were deemed benign.
According to the results, the presence of polygonal shape (p = 0.005 and p = 0.019 for reviewers 1 and 2, respectively) peripheral subpleural lesion (p = 0.011 and p = 0.033), a predominantly solid lesion (p < 0.001 and p < 0.001) and 3D ratios (p < 0.011 and p < 0.001) were greater in benign lesions than in atypical adenomatous hyperplasias.
"When we used a single CT feature, the highest accuracy (85% and 89% for reviewers 1 and 2, respectively) was obtained with a predominantly solid lesion for both reviewers," the authors wrote. "However, specificity of the predominantly solid lesions was limited (78% and 84%, respectively, with six false-positive results). Concave margins were seen in 19 ... of the 40 benign lesions, two of seven atypical adenomatous hyperplasias, and two ... of the 25 malignant lesions."
Meanwhile, polygonal shape was completely specific to benign lesions (100% for both reviewers), but its sensitivity (28% and 20% for the two reviewers, respectively) was low. In addition, the presence of a peripheral subpleural lesion was greater in atypical adenomatous hyperplasias than in malignancies, the authors wrote.
Combining two nodule features at a time, a predominantly solid lesion paired with a peripheral subpleural lesion yielded 100% specificity but just 30% sensitivity for benignity between the two readers. Combining a peripheral subpleural lesion with a predominantly solid pattern was 100% specific and 53% sensitive for benignity between the two readers.
As for limitations, the study cohort reflected a largely rural Japanese population at low risk for lung cancer, resulting in a high prevalence (44%) of bronchioalveolar carcinoma among the cancers detected. In comparison, only 11% of the cancers were bronchioalveolar in a U.S. study conducted by Dr. Claudia Henschke, the authors stated (The Lancet, July 10, 1999, Vol. 354:9173, pp. 99-105).
Thus, 43% of participants in the Japanese study were nonsmoking women, and only 16% were smokers of 10 pack years or more.
"Tobacco smoke is closely related to squamous cell carcinoma and small cell carcinoma, but is far less related to bronchioalveolar carcinoma," the authors stated. "This, combined with the low prevalence of tuberculosis, may explain the low frequency of nodules smaller than 3 mm."
Another limitation of the study was seen in the two-year stability criteria for nodules, which has recently come under criticism due to the rapid growth of some cancers.
"Nonetheless, our study seems to indicate that high-resolution CT analysis is helpful in managing cases with small solitary pulmonary nodules discovered at population-based CT screening for lung cancer," Takashima and colleagues wrote. "Such analysis may contribute to obviating follow-up CT and invasive diagnostic procedures in patients with small benign nodules in the lung."
By Eric BarnesAuntMinnie.com staff writer
April 29, 2003
Related Reading
Pros and cons of widespread CT lung cancer screening still debated, March 12, 2003
Lung CAD applications starting to outread radiologists, February 13, 2003
Ground-glass lung lesions on CT are treatable with limited excision, February 10, 2003
Lung cancer screening not cost-effective, say Johns Hopkins researchers, January 14, 2003
Why CT lung cancer screening will (and won't) work, November 11, 2002
Copyright © 2003 AuntMinnie.com