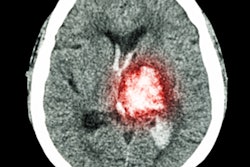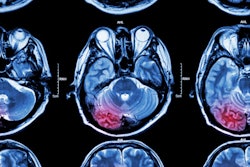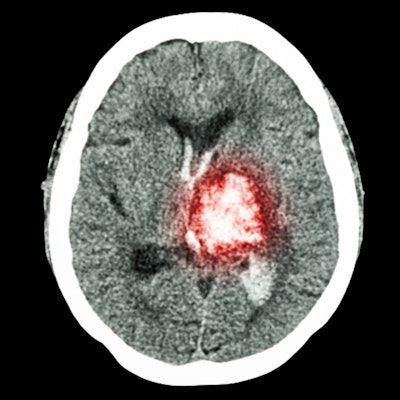
The combination of standard noncontrast CT and CT perfusion can identify which stroke patients are likely to benefit from surgical treatment better than either of the modalities alone, according to a study recently published online in Annals of Neurology.
The researchers, led by Dr. Amrou Sarraj from the University of Texas at Houston, examined the clinical management of 361 stroke patients as part of an ongoing multicenter study. All of the patients underwent standard CT and CT perfusion to determine if they would benefit from endovascular thrombectomy. Patients whose standard CT and CT perfusion scans indicated a favorable outcome after surgery were nearly four times more likely to receive surgical treatment (Ann Neurol, January 9, 2020).
The group discovered that 58% of patients with a favorable profile on both standard CT and CT perfusion achieved functional independence within the first 90 days after surgery. This percentage was considerably greater than the 38% surgery success rate when only one of the modalities indicated a favorable profile and the 0% success rate when neither of the modalities indicated a favorable outcome.
"While best outcomes were observed in patients with a favorable profile on both imaging modalities, patients who had a favorable profile on at least one imaging modality also achieved reasonable outcomes," Sarraj said in a university statement.