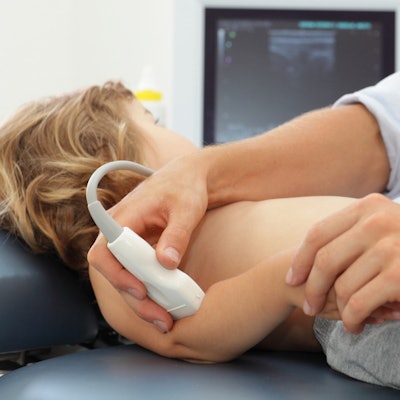
Ultrasound performs just as well as MRI for musculoskeletal (MSK) indications, suggesting that a follow-up MRI scan after an initial ultrasound exam may be unnecessary, according to research published online May 5 in the Journal of the American College of Radiology.
Previous studies have shown that ultrasound can offer comparable, complementary, or even superior results to MRI for evaluating MSK symptoms, wrote a team led by Dr. Lulu He of Mercy Fitzgerald Hospital in Darby, PA. But in the U.S., MRI is still considered the gold standard, and ultrasound is underused, despite its accessibility and lower cost.
Mercy Fitzgerald has a thriving MSK ultrasound practice, the group wrote. When the practice's medical director observed that MRI exams were often ordered and performed after diagnostic ultrasound examinations had been conducted for the same clinical concerns -- and questioned whether these follow-up MRI scans added any diagnostic value -- He and colleagues tested the hypothesis that MSK ultrasound examinations produce results comparable to those obtained with MRI.
The group included data from 129 MRI exams performed within 90 days of diagnostic musculoskeletal ultrasound between January 2012 and November 2015. Two MSK radiologists independently compared the ultrasound and MRI reports, categorizing their impressions as concordant (no or minor difference between results) or discordant (potentially clinically important difference between results).
The two readers agreed on concordance or discordance between ultrasound and MRI findings in 124 of 129 cases. There were 16 discordant reports (12%); image review of both modalities showed image agreement for 11 of the 16 and disagreement in the remaining five in both reports and images.
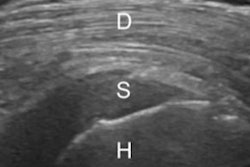
The most common reasons for report disagreement despite image agreement between the two modalities were wording variations and differences in reader interpretation of imaging findings. When the two exams did not agree in both report and imaging findings, the most common reason was due to inappropriate use of the initial ultrasound exam, such as with masses larger than 5 cm and/or deep to the superficial muscular fascia, the researchers found.
Yet, overall, the study found high concordance between ultrasound and follow-up MRI exam reports (88%) and images (96%) for a range of musculoskeletal indications. In fact, only 2% of cases from the study period fit inclusion criteria, reflecting a lower incidence of redundant imaging than the group had expected. The team attributed this to ongoing efforts to educate physicians on the proper use of ultrasound exams and also radiologist guidance as to ultrasound's suitability for the indication at the time the exam was ordered.
"[An] appropriately ordered MSK ultrasound examination can serve as a definitive advanced imaging modality, limiting the need for an additional MRI examination," the authors concluded.




![Overview of the study design. (A) The fully automated deep learning framework was developed to estimate body composition (BC) (defined as subcutaneous adipose tissue [SAT] in liters; visceral adipose tissue [VAT] in liters; skeletal muscle [SM] in liters; SM fat fraction [SMFF] as a percentage; and intramuscular adipose tissue [IMAT] in deciliters) from MRI. The fully automated framework comprised one model (model 1) to quantify different BC measures (SAT, VAT, SM, SMFF, and IMAT) as three-dimensional (3D) measures from whole-body MRI scans. The second model (model 2) was trained to identify standardized anatomic landmarks along the craniocaudal body axis (z coordinate field), which allowed for subdividing the whole-body measures into different subregions typically examined on clinical routine MRI scans (chest, abdomen, and pelvis). (B) BC was quantified from whole-body MRI in over 66,000 individuals from two large population-based cohort studies, the UK Biobank (UKB) (36,317 individuals) and the German National Cohort (NAKO) (30,291 individuals). Bar graphs show age distribution by sex and cohort. BMI = body mass index. (C) After the performance assessment of the fully automated framework, the change in BC measures, distributions, and profiles across age decades were investigated. Age-, sex-, and height-adjusted body composition reference curves were calculated and made publicly available in a web-based z-score calculator (https://circ-ml.github.io).](https://img.auntminnie.com/mindful/smg/workspaces/default/uploads/2026/05/body-comp.XgAjTfPj1W.jpg?auto=format%2Ccompress&fit=crop&h=100&q=70&w=100)





![Overview of the study design. (A) The fully automated deep learning framework was developed to estimate body composition (BC) (defined as subcutaneous adipose tissue [SAT] in liters; visceral adipose tissue [VAT] in liters; skeletal muscle [SM] in liters; SM fat fraction [SMFF] as a percentage; and intramuscular adipose tissue [IMAT] in deciliters) from MRI. The fully automated framework comprised one model (model 1) to quantify different BC measures (SAT, VAT, SM, SMFF, and IMAT) as three-dimensional (3D) measures from whole-body MRI scans. The second model (model 2) was trained to identify standardized anatomic landmarks along the craniocaudal body axis (z coordinate field), which allowed for subdividing the whole-body measures into different subregions typically examined on clinical routine MRI scans (chest, abdomen, and pelvis). (B) BC was quantified from whole-body MRI in over 66,000 individuals from two large population-based cohort studies, the UK Biobank (UKB) (36,317 individuals) and the German National Cohort (NAKO) (30,291 individuals). Bar graphs show age distribution by sex and cohort. BMI = body mass index. (C) After the performance assessment of the fully automated framework, the change in BC measures, distributions, and profiles across age decades were investigated. Age-, sex-, and height-adjusted body composition reference curves were calculated and made publicly available in a web-based z-score calculator (https://circ-ml.github.io).](https://img.auntminnie.com/mindful/smg/workspaces/default/uploads/2026/05/body-comp.XgAjTfPj1W.jpg?auto=format%2Ccompress&fit=crop&h=112&q=70&w=112)








