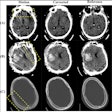
CHICAGO - When typical CT features of pancreatic malignancy are present, there's no need for percutaneous biopsy, according to the results of a five-year study at a London hospital. As always, oncologists and patients may be hesitant to stop after imaging alone, but the additional information gleaned from biopsy could help direct patient management if other factors, particularly age, are taken into account.
The retrospective study, presented at the RSNA meeting Monday by Dr. William Lees from University College London, included 303 patients (ages 26-89) who underwent percutaneous biopsy with an 18-gauge Trucut powered cutting needle. All patients showed a pancreatic mass at CT, with corroborating findings at MRI, ultrasound, or endoscopic retrograde cholangiopancreatography (ECRP), suggesting the need to biopsy for a pancreatic cancer diagnosis.
The purpose of the study was twofold: to determine the yield and success rate of the percutaneous biopsy method, and to establish the sufficiency of CT criteria for diagnosing pancreatic malignancy.
"We studied all biopsies and CT scans performed over a five-year period up to 2003," Lees said. "We established our typical CT criteria for ductal adenocarcinoma, which as you know (represents) 90% of pancreatic malignancy."
Typical CT features suggestive of pancreatic adenocarcinoma included:
- Poorly enhancing mass seen in the parenchymal phase
- Biliary or pancreatic dilation
- Vascular infiltration
- Infiltration of peripancreatic fat
Atypical features included:
- Presence of calcification
- A hyper- or iso-enhancing mass
- Rim enhancement
- Absence of duct dilatation or uniduct dilatation
- Cystic change
All patients underwent pancreatic biopsy except for those considered operable, and the final diagnosis was based on histology, or at least six months of clinical and radiological follow-up in cases of negative biopsy, Lees said. Most patients (n = 247) had only one biopsy, 45 had two biopsies, and one 26-year-old patient underwent five biopsies before the doctors were satisfied with his negative diagnosis. Most procedures were guided by ultrasound, others by CT, and a few with ultrasound and fluoroscopy, he said.
"We almost always visualize the mass on ultrasound, which is very effective in demonstrating the size and distribution of the tumor mass, and recently we've been using ultrasound contrast agents, which enhance the conspicuity of the mass."
According to the results, 240 of 303 patients had a histological diagnosis of ductal adenocarcinoma, 10 had neoendocrine tumors, and 13 other tumor types over the five-year period. The percutaneous procedure had a 90% sensitivity (70% for the initial biopsy alone) and 100% specific for malignancy. Most complications (n = 14) were minor except for three (0.8%), which included an abscess, a duodenal perforation, and a significant retroperitoneal bleed, Lees said. There were no cases of tumor seeding as a result of the biopsies.
The typical CT features enabled a specific diagnosis of ductal adenocarcinoma in 68% of patients, with specificity of 95% and a positive predictive value of 98%. Atypical features had a negative predictive value of 41%.
"The 18-gauge Trucut biopsy is highly sensitive and specific for the diagnosis of pancreatic malignancy; our pathologists are completely happy to diagnose any particular tumor," Lees said.
His group believes the safety profile of biopsies is adequate. Also, the CT features of ductal adenocarcinoma have a high positive predictive value of over 98%, he said.
Based on the results, "I'm proposing that in our institution, which is a tertiary referral practice for pancreatic cancer, biopsy can be omitted if you have typical features, particularly in the elderly, which is a big chunk of patients presenting for treatment. I think we can probably drop 30% of our biopsies with an error rate of less than 2%," Lees said.
Oncologists are extremely unhappy about treating patients without a tissue diagnosis, said one audience member. Lee agreed, noting that most patients with a positive diagnosis are sent on to chemotherapy, "which is useless."
Age is a key factor that might enable a reduction in biopsies, Lee said, most patients are age 60 and older. Younger patients, and those who are being considered for extensive radiochemotherapy treatments, will likely continue to undergo biopsies, he said.
By Eric Barnes
AuntMinnie.com staff writer
November 28, 2005
Related Reading
3D MRI spots small pancreatic cancers, September 15, 2005
High-intensity focused ultrasound shows promise in pancreatic cancer, August 30, 2005
Fruit, veggies tied to lower pancreatic cancer risk, April 4, 2005
Copyright © 2005 AuntMinnie.com