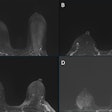
Computer-aided detection (CAD) continues to prove itself as the technology that is most likely to succeed in taking mammography to the next level. Clinical studies bolster CAD's ability to catch about 20% more tumors or suspicious areas, resulting in more accurate reads, better recommendations for follow-up studies, and fewer unnecessary biopsies.
The most recent study by Dr. Rachel Brem and colleagues at George Washington University Medical Center in Washington, DC, called CAD a useful tool to prompt the radiologist to identify potential areas of abnormality on the mammogram (Cancer, September 1, 2005, Vol. 104:5, pp. 931-935).
Previously, Dr. Robyn Birdwell and colleagues at Stanford University Medical Center in Stanford, CA, found that the prospective clinical use of CAD in a university hospital setting resulted in a 7.4% increase in cancers detected (Radiology, August 2005, Vol. 236:2, pp. 451-457).
And Italian investigators compared two CAD systems and concluded that both produced an increase in overall sensitivity, with a little decrease in specificity, when used as a second reader (European Journal of Radiology, August 2005, Vol. 55:2, pp. 264-269).
Despite these positive results, from the malpractice insurance underwriting perspective, CAD does not have enough of a track record. Without that historical data, it is unlikely that insurance carriers will want to justify premium credits or a revision of rates. So how does an underwriter determine if a new technology merits an overhaul of their current policies?
First, insurance companies do not consider new technologies until it directly affects their bottom line over a significant period of time -- it takes many years of changes in loss experience for them to recognize other avenues. Even then, premium decreases are not based on the technology use, but the reduced frequency and severity of claims in a large section of the specialty. Again, this has to take place over a number of years. In addition, claims managers and attorneys must confirm that the technology is indeed responsible for the improved loss experience.
Here are some of the concerns that prominent radiology underwriters currently have about using CAD in mammography:
What degree of training is sufficient for adequately training radiologists on CAD? Underwriters need to know that any training standards set by organized radiology are considered mandatory or sufficient. A recent study from Europe found that pairing CAD with a mammography workstation allowed for efficient soft-copy reading for detecting microcalcifications. A second report tested a CAD training program with a cognitive-perceptual-based hypermedia program. The researchers determined that "CAD training will influence the perception, recognition, and interpretation of early breast cancer and CAD performance studies" (European Radiology, August 25, 2005; Academic Radiology, August 2005, Vol. 12:8, pp. 1039-1048).
Also, quality assurance (QA) is a big issue. How does a practice ensure that CAD is being used properly? Are exams overread during random internal checks, or is an outsider brought in for QA control? A small number of groups actually employ radiologists whose sole job is QA, in terms of exam quality, the quality of reads, and the accuracy of the reports.
If a facility or radiologist chooses not to use CAD, can the facility, radiologists, and/or referring physician be held responsible for not using the most advanced technology available?
On a similar note, a radiologist may be found liable for depriving a patient of the most advanced form of technology, especially if it has been proved to increase accuracy and is widely available.
- Ideally, patients should be notified if CAD will not be used for mammographic interpretation and be given the option to schedule an appointment at a breast imaging center that does. However, the patient must be clear on the negative consequences of such a decision -- for example, a long wait time for an appointment, longer wait for results, and perhaps greater travel distance. Needless to say, delaying an exam for the sake of advanced technology is ill advised.
While CAD has been shown to improve accuracy of interpretation, does this mean that exams in which CAD was used must be held to a higher standard versus a traditional mammographic interpretation? Underwriters and claims attorneys believe CAD exams should be held to a higher standard, in which case CAD can be used for or against a radiologist. The general opinion is that it is more likely to work in the radiologist's favor.
Improved accuracy will most likely reduce the number of claims filed. But an increase in the severity, or amount, of claims paid is also likely in the event a court is convinced the radiologist has caused harm to the patient. Anytime a physician is considered an "expert" in a certain field, and medical equipment or technology is considered to be far above the norm, all are held to a higher standard.
It's impossible to predict how this will play out, as each case will be different. But a well-trained, experienced radiologist who reads a significant number of breast exams, and uses CAD, is far more likely to make an accurate read than one who does not have adequate training or experience, at least in the underwriter's estimation.
A common thread here is the legal concerns about CAD's role in breast imaging, the most litigated field within radiology. Misread mammograms continue to be the leading cause of claims against radiologists, and often result in the highest monetary payouts.
But that dark legal cloud that looms over mammography doesn't necessarily mean disaster is imminent. Advances such as CAD is a first step to sheltering mammography from rack and ruin, and any improvements in interpretation of breast imaging is a very good thing.
Two insurance underwriters that I spoke with compared mammography's quandary with that of anesthesiology's in the late 20th century. In the 1970s and 80s, malpractice premiums in that field were the highest and many insurers refused to insure anesthesiologists at all.
But with the introduction and adoption of pulse oximetry and capnography, as well as improvements in training, anesthesiology is now considered one of the least hazardous specialties. Both methods are considered mandatory for meeting the standards of care. In fact, the majority of malpractice insurance carriers will not insure anesthesiology if they do not use pulse oximetry and capnography.
The size of payments from successful malpractice suits against anesthesiologists also has declined. According to the American Society of Anesthesiologists, the median payment during the 1970s was $332,280. By the 1990s, it had dropped to $179,010.
This dramatic reduction in malpractice premiums resulted from an industry-wide effort by the anesthesiology community and equipment manufacturers in general to produce hard data proving that the new technology made a significant difference.
Mammographers need to do the same with CAD. Radiology practices utilizing CAD should consider the following:
Keep detailed data on claims involving CAD reads versus traditional mammogram reads.
It is imperative that radiologists and technologists are thoroughly trained in the use of CAD, including an understanding of how CAD reads differ from non-CAD.
Compare missed cancer from normal mammograms to those read by CAD, as well as the exam details, such as the technologist who performed the exam and the radiologist who did the read. Was the quality of the mammogram up to standards? Should another exam have been ordered?
Manufacturers can assist by making "plain language" demonstrations that show how CAD works, with explanations of how the new technology differs from the old. It takes a well-versed radiologist to explain to a patient or other nonmedical person how CAD works, what the markings means, and how they can affect interpretation and follow-up recommendations.
Get involved with insurance brokers who understand imaging to call underwriters' attention to the advantages of CAD.
Most insurance underwriters will take a lot of convincing. But there are some out there who are open to new technology and, most importantly, how those advances can reduce the potential for claims.
By T. Lloyd Croft
AuntMinnie.com contributing writer
October 21, 2005
T. Lloyd Croft is a vice president of Professional Medical Insurance Services. He is based in Arlington Heights, IL.
Related Reading
CAD marks: To save or not to save? September 1, 2005
CARS panel discusses the future of CAD, June 28, 2005
Copyright © 2005 AuntMinnie.com