TORONTO - MRI shows that antiretroviral therapy use is tied to fat deposition in people living with HIV, according to research presented June 4 at the International Society for Magnetic Resonance in Medicine (ISMRM) annual meeting.
In her presentation, Patricia Maishi from the University of Cape Town in South Africa found through the use of cardiovascular MR that people living with HIV who undergo such therapy have increased pericardial adipose tissue and paracardiac adipose tissue compared with those who are uninfected.
"We wanted to investigate this population and how antiretroviral therapy affects their wellbeing," Maishi told AuntMinnie.com. "We're seeing most of the images we take have a pericardial effect. We wanted to count participants before they can show the signs of cardiovascular disease."
Cardiovascular disease is a major contributor to morbidity and mortality in people living with HIV. Increased pericardiac adipose tissue is linked to poor cardiovascular outcomes in the general population. However, Maishi, a senior MR radiographer at the University of Cape Town, noted that its role in HIV-associated cardiovascular disease is not well described.
She also reported that South Africa has the largest HIV epidemic in the world, with 8.2 million people in the country having the disease. While widescale availability of antiretroviral therapy has decreased the number of deaths from HIV, previous research suggests that it may also be tied to cardiovascular disease. This includes heart failure with preserved ejection fraction, myocardial inflammations, and myocardial fibrosis among others.
Maishi and colleagues wanted to study such prevalence in people living with HIV who also undergo antiretroviral therapy use. They wanted to quantify pericardial adipose tissue and paracardiac adipose tissue in patients by using 3T cardiovascular MRI. Additionally, they wanted to explore the potential relationships between these tissues and other factors such as HIV disease duration, therapy regimen, deformational characteristics, inflammation, and fibrosis.
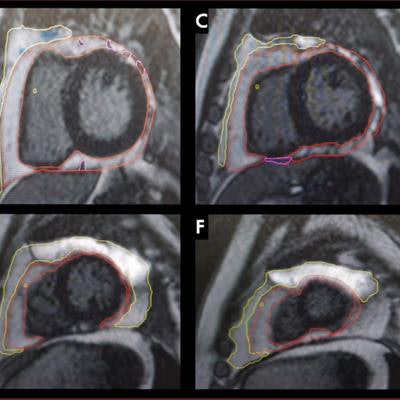
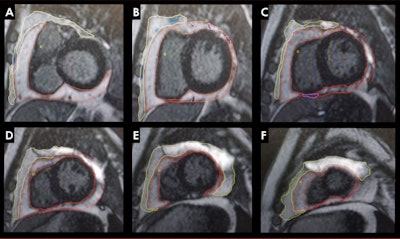 Patricia Maishi presented findings from her team's award-winning study at the ISMRM annual meeting showing ties between antiretroviral therapy use in people living with HIV and adipose deposition affecting cardiac health. The yellow outline represents paracardiac fat volumes while the red outline represents pericardial fat volumes. Image courtesy of Patricia Maishi.
Patricia Maishi presented findings from her team's award-winning study at the ISMRM annual meeting showing ties between antiretroviral therapy use in people living with HIV and adipose deposition affecting cardiac health. The yellow outline represents paracardiac fat volumes while the red outline represents pericardial fat volumes. Image courtesy of Patricia Maishi.The team included data from 198 patients. Of these, 131 were living with HIV and undergoing antiretroviral therapy, 19 were living with HIV but not undergoing therapy, and 48 were healthy controls.
The researchers found that the therapy group had significantly higher levels of both pericardial adipose tissue and paracardiac adipose tissue compared to the nontherapy and healthy control groups.
| Comparison between groups for fat tissue deposition | ||||
| Characteristic median | Control group | Nontherapy group | Therapy group | p-value |
| Pericardial adipose tissue, ml | 23.01 | 32.1 | 43.1 | < 0.001 |
| Pericardial adipose tissue, ml/m² | 5 | 19.5 | 24.2 | < 0.001 |
| Paracardiac adipose tissue, ml | 0 | 0 | 9 | < 0.001 |
| Paracardiac adipose tissue, ml/m² | 0 | 0 | 5 | < 0.001 |
The researchers also found that the therapy group and non-therapy groups had higher left ventricular mass than the healthy control group while the control group had higher right ventricular ejection fraction than both HIV groups.
The team also reported that both HIV groups had higher extracellular volume, T1 and T2 times, and late gadolinium enhancement than the control group. However, the nontherapy group had the highest measures of the three groups. Maishi said this indicates that despite higher volumes of fat deposition for the therapy group, the nontherapy HIV group experiences greater effects of inflammation.
Maishi also said that both pericardial and paracardiac adipose tissues showed weak correlations with indicators of myocardial function and tissue characteristics. She told AuntMinnie.com that future studies could investigate what causes right ventricular dysfunction in the HIV groups.
This research received the president's award from the International Society for MR Radiographers & Technologists (ISMRT), a section of the ISMRM.















![Overview of the study design. (A) The fully automated deep learning framework was developed to estimate body composition (BC) (defined as subcutaneous adipose tissue [SAT] in liters; visceral adipose tissue [VAT] in liters; skeletal muscle [SM] in liters; SM fat fraction [SMFF] as a percentage; and intramuscular adipose tissue [IMAT] in deciliters) from MRI. The fully automated framework comprised one model (model 1) to quantify different BC measures (SAT, VAT, SM, SMFF, and IMAT) as three-dimensional (3D) measures from whole-body MRI scans. The second model (model 2) was trained to identify standardized anatomic landmarks along the craniocaudal body axis (z coordinate field), which allowed for subdividing the whole-body measures into different subregions typically examined on clinical routine MRI scans (chest, abdomen, and pelvis). (B) BC was quantified from whole-body MRI in over 66,000 individuals from two large population-based cohort studies, the UK Biobank (UKB) (36,317 individuals) and the German National Cohort (NAKO) (30,291 individuals). Bar graphs show age distribution by sex and cohort. BMI = body mass index. (C) After the performance assessment of the fully automated framework, the change in BC measures, distributions, and profiles across age decades were investigated. Age-, sex-, and height-adjusted body composition reference curves were calculated and made publicly available in a web-based z-score calculator (https://circ-ml.github.io).](https://img.auntminnie.com/mindful/smg/workspaces/default/uploads/2026/05/body-comp.XgAjTfPj1W.jpg?auto=format%2Ccompress&fit=crop&h=112&q=70&w=112)




