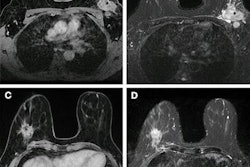
Imaging will have a key role in managing infectious and inflammatory breast lesions, according to consensus guidelines published April 1 in JAMA Surgery.
Among other care considerations and management strategies, the guidelines highlight how ultrasound and mammography can help with diagnosing mastitis. The guidelines provide management recommendations for lactational, granulomatous, and periductal mastitis with squamous metaplasia of lactiferous ducts (PDM-SMOLD).
The following medical societies developed the guidelines: the American Society of Breast Surgeons, the Society of Breast Imaging, and the College of American Pathology.
“The treatment pathways outlined herein reflect movement toward minimally invasive interventions and utilization of adjunctive medical therapies for disease resolution, although some infectious entities still require an operative procedure for resolution,” the societies stated.
The latest guidelines are the second installment of guidelines by the three societies on managing benign breast disease. The societies noted that managing mastitis has “significantly changed” over the last 10 years.
“We prioritized management of lactational mastitis, granulomatous mastitis, and PDM-SMOLD because of the controversial management of these conditions and the lack of existing guidelines on these conditions,” they wrote.
Lactational mastitis
The societies reported having “strong consensus” for the following recommended imaging strategies at the time of diagnosis:
Ultrasound for patients with infectious lactational mastitis with a breast mass and cellulitis at presentation.
Ultrasound for patients with infectious lactational mastitis with cellulitis whose cases do not resolve with medical or symptom management.
Mammograms for patients with lactational mastitis if the symptoms are refractory to treatment. This is to rule out a malignancy or if the patient (when comfortable) qualifies for age-appropriate screening.
Granulomatous mastitis
The societies also reached “strong consensus” on the following imaging recommendations at a time of diagnosis:
Ultrasound for patients at first presentation to aid with treatment planning. Mammograms for suspicious findings to rule out malignancy.
Consider follow-up imaging during treatment if there is symptom progression.
While not the recommended standard imaging method, breast MRI could also show nodular lesions with ring enhancement and “can give a more accurate picture of the extent of disease,” the guideline authors highlighted.
PDM-SMOLD
The societies also achieved “strong consensus” for the following imaging recommendations at a time of diagnosis:
Ultrasound for all patients initially presenting with PDM-SMOLD.
Repeat ultrasound if condition does not improve after one to two weeks after initial course of antibiotics.
Consider mammography for patients ages 30 or older and have discordant ultrasound findings or patients who don’t respond to treatment after one to two weeks to rule out a malignancy.
When available, ultrasound guidance for aspirations of fluid collections for PDM-SMOLD.
The guideline authors suggested that future directions will include exploring new agents that can be applied to treating granulomatous mastitis and gaining more insight into prevention of PDM-SMOLD.
“Clinicians can use these guidelines to appropriately manage these conditions for which clinical care often varied in the past,” they wrote.
Read the full statement here.