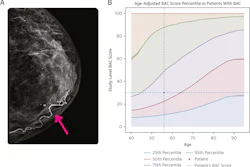
Two U.S. Food and Drug Administration (FDA)-cleared AI algorithms show promise for prioritizing high-risk screening mammograms for same-day diagnostic evaluation, researchers have reported.
A team led by Diana L. Miglioretti, PhD, of the University of California, Davis, found that the tools identified half of all screen-detected cancers while flagging just 2% of exams. The study results were published May 2 in the Journal of the American College of Radiology.
"Our findings support a clinically feasible strategy in which AI is used to triage a limited number of screening mammograms for immediate remote interpretation, enabling same-day diagnostic mammography for patients most likely to benefit (i.e., those with cancer visible at screening) and potentially decreasing the time to diagnostic resolution," the group wrote.
Regular screening mammography reduces breast cancer mortality, but in the U.S., more than 3.8 million individuals are recalled for suspicious findings, the team explained, noting that "because diagnostic evaluation typically requires at least one additional visit, recalls can lead to delays in diagnostic resolution, anxiety, financial and opportunity costs, and loss to follow-up," challenges that "disproportionately affect under-resourced and rural populations."
One approach to reducing diagnostic delays is immediate interpretation of screening exams while patients wait. But this can be hard to implement, according to the group. AI algorithms used with screening mammography could help identify exams with suspicious findings and support targeted, immediate interpretation workflows.
Miglioretti and colleagues conducted an analysis of 3,468 screening digital breast tomosynthesis exams and applied two FDA-cleared AI algorithms (iCAD Profound version 0.2.0.2, or "AI1," and Lunit Insight DBT v1.0.0.2, or "AI2") using the ClinValAI framework to generate exam-level malignancy suspicion scores.
Of 3,468 screening mammograms, 213 (6.1%) were recalled, and within one year of screening, 25 breast cancers were diagnosed (7.2 out of 1,000). Twenty were detected following a positive screening mammogram (cancer detection rate 5.8 out of 1,000), and five were diagnosed within one year of a negative screening mammogram (false-negative rate 1.4 out of 1,000).
The team found the following:
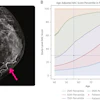
- The two AI algorithms showed comparable performance, with modest discrimination for identifying mammograms recalled for additional imaging (AUC AI1, 0.676, and AI2, 0.670).
- They showed excellent discrimination for identifying mammograms with screen-detected cancer (AUC AI1, 0.952, and AI2, 0.908) and cancers diagnosed within a year (AUC AI1, 0.852 and AI2, 0.907).
- Mammograms in the highest 2% of AI scores captured 7.5% to 9% of all recalls and 50% of all screen-detected cancers.
In light of the study results, Miglioretti and colleagues suggested that AI could flag high-suspicion examinations for priority image upload and immediate remote interpretation, potentially enabling same-day diagnostic mammography.
Access the full study here.