A 13-year-old girl, resident of Pune, presented with insidious onset of yellowish discoloration of eyes and urine for one year and painless distension of abdomen for last six months associated with progressive altered sensorium for 15 days.
There were features of dysphagia, dysarthria, dystonia, chorea, and cognitive decline with recent worsening in the form of altered sensorium, fever, and coagulopathy. Over the year, she gradually developed involuntary, nonrepetitive, purposeless movement of all four limbs. She was noticed to have yellow discoloration of urine and eyes, which was associated with right upper quadrant pain and loss of appetite.
There was no history of pruritus, clay-colored stool, haematemesis, melaena, skin rash, easy bruisability, or abnormal behaviour. There was no history of weakness of limbs, trunk or respiratory muscles, or sensory phenomena. There was no history of jaundice in any other family members.
General examination revealed thinly built, poorly nourished febrile, icteric young girl with pedal edema and gum bleeding. Slit lamp exam of eyes showed Kayser Fleischer ring. Systemic examination performed, revealed evidence of coma, with GCS: E4M3V1: 8/15. There was generalised wasting with rigidity of all four limbs, associated with normal tendon jerks and extensor plantars response bilaterally.
Abdomen evaluation showed splenomegaly with ascites. The abnormal laboratory investigations included elevated serum bilirubin 3.3 mg/dl, prolonged Prothrombin time (control 12 and test 26 seconds), PTTK (control 32 and test 36 seconds). The serum ceruloplasmin measured 75 IU/L (normal values: 500-1000 IU/L) while serum copper values were 30.6 ug/dl (normal values: 70-140 ug/dl). The EEG findings were suggestive of diffuse cerebral dysfunction with no evidence of epileptiform discharges.
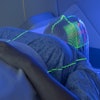
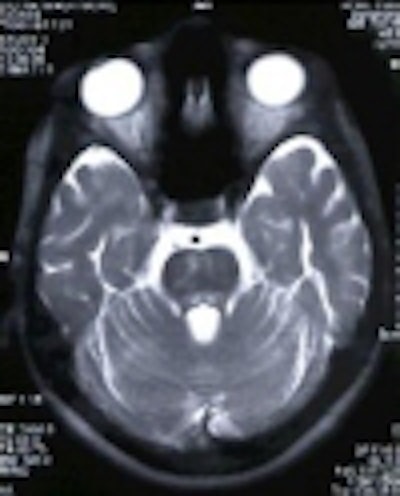
MRI was performed with the following sequences: TSE and gradient-echo T2 and FLAIR axial, TSE T2 sagittal and coronal, 3D Turboflash T1 sagittal with multiplanar reconstructions, and diffusion-weighted images with b-values of 500 and 1000 s/sq mm.
Key findings on MRI
There was symmetrical hyperintensity at both putamina and thalami and the head of both caudate nuclei on T2WI and FLAIR images [Figure 1 and 2]. The thalamic lesions appear hypointense on T1WI while the putaminal lesions show mixed signal with magnetic susceptibility effects on gradient-echo images.
Figure 1
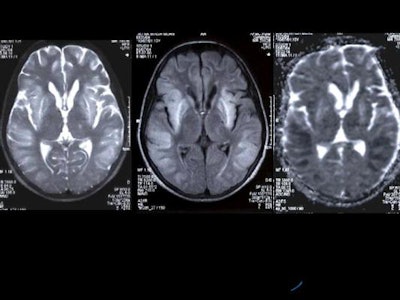 |
Figure 2
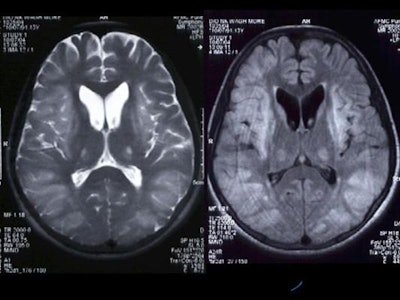 |
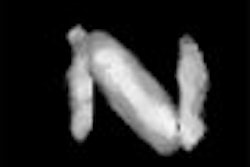
Hyperintensity was also present in the posterior pons and quadrigeminal plate on T2W and FLAIR images, appearing mildly hypointense on T1WI. [Figure 3]
Figure 3
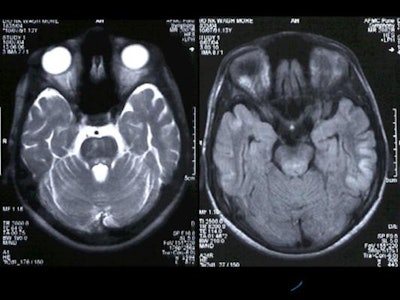 |
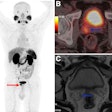
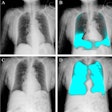
Diffuse hyperintensity at the cortex of both cerebral hemispheres on T2W and FLAIR images, with sparing of the white matter, was present [Figure 4]. These regions appeared mildly hypointense on T1WI. Mild sulcal effacement is seen in the involved regions.
Figure 4
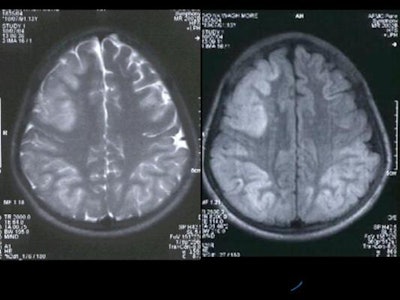 |
On diffusion-weighted images, there were hyperintense signals in the basal ganglia which appeared hyperintense on ADC maps, which implied that there was no restriction of diffusion in basal ganglia. However, the cortical grey matter showed hyperintense signals which appeared hypointense on ADC maps which indicated true restriction of diffusion [Figure 5].
Figure 5
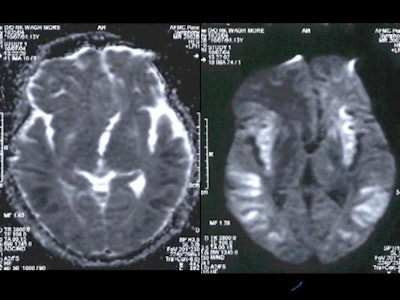 |
Gradient-echo images showed hypointensities in the region of basal ganglia suggestive of metal deposition [Figure 6].
Figure 6
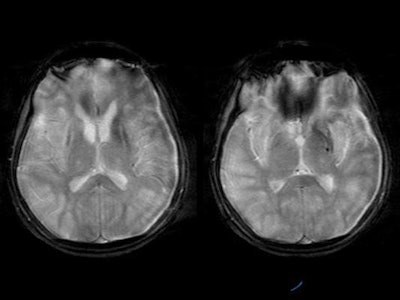 |
Based on the MRI the following observations were made:
- Changes in the basal ganglia and thalami were consistent with Wilson’s disease.
- The diffuse cortical lesions with relative sparing of the white matter was considered of recent onset and attributed to one of the possibilities mentioned below:
- Further progression of Wilson’s disease.
- Hepatic failure as a part of portosystemic encephalopathy.
- Drug toxicity.
The patient was subsequently placed on treatment tab penicillamine 250 mg BD, and is currently on follow-up. A repeat MRI is scheduled during her follow-up.
Final diagnosis
Wilson’s disease involving basal ganglia, pons, and cerebral cortex
Discussion
Wilson’s disease is an autosomal recessive condition characterised by defective copper metabolism (AJR, December 1996, Vol. 167:6, pp. 1579-1584). The hallmark of this condition is a deficiency in serum ceruloplasmin, which results in abnormal accumulation of copper, a heavy metal, in the liver initially and subsequently in the brain and other organs. The definitive diagnosis of this condition is established by measuring serum levels of ceruloplasmin and copper.
In Wilson’s disease, clinically the liver manifestations comprise acute, chronic, and fulminant hepatitis, portosystemic collaterals and other manifestations of cirrhosis, while the neurological involvement is characterised by neurodegenerative changes involving the basal ganglia and thalami.
There are three subgroups of neuropsychiatric symptoms based on the anatomical location of lesion. The first subgroup presents with bradykinesia, rigidity, cognitive impairment, and an organic mood syndrome with an MRI correlation of a dilated third ventricle. The second subgroup has ataxia, tremor, and reduced functional capacity with focal thalamic lesions. The third subgroup has dyskinesia, dysarthria, and an organic personality syndrome, with demonstrable focal lesions in the putamen and pallidum (Neurology, January 1993, Vol. 43:1, pp. 120-124).
The MR appearances of brain lesions in Wilson’s disease have been well documented. The lesions have been documented in the following areas by various authors (AJR, December 1996, Vol. 167:6, pp. 1579-1584; Neurology, January 1993, Vol. 43:1, pp. 120-124; Acta Radiologica, March 1997, Vol. 38:2, pp. 250-258):
- Basal ganglia (putamen, globus pallidus, caudate nucleus, thalamus and sub thalamus)
- Midbrain (tegmentum, substantia nigra, red nuclei, inferior tectum and crura)
- Pons (dorsal and ventral)
- Cerebellum (superior, middle peduncles and dentate nuclei)
- Cerebral white matter (frontal lobe commonly)
- Cerebral cortex
Notwithstanding the above classical features, in recent times there have been numerous publications highlighting uncommon and atypical presentations (AJR, October 1998, Vol. 151:4, pp. 834). In our case the cortical involvement was extensive.
There is, in addition, a specific sign for the lesions of pons and midbrain, widely termed as "face of giant panda" and "cub of giant panda" signs. On MRI, the lesions reveal bilaterally symmetric increased T2 signal intensity in most of the locations described above, which signifies gliosis and/or edema.
Diffusion-weighted imaging is increasingly applied in cases of Wilson’s disease. In a recent study, diffusion MRI was performed on four patients with Wilson's disease, which showed abnormal high signals on ADC maps in some areas of the basal ganglia in. The authors also ascribe regions of low signal on T2-MRI to copper deposits, and abnormal high signal on diffusion MRI to parenchymal lesions such as cell loss, demyelination and/or increase of the extracellular fluid (Rinsho Shinkeigaku, April 1993, Vol. 33:4, pp. 446-448).
It is also established that lesions of cortex and white matter are present in approximately 10% of cases. One recent reported case of Wilson's disease was diagnosed after an episode of partial motor epileptic seizures. MRI in this case revealed cortical and subcortical lesions by an enhanced signal (T2 values), besides the classical picture of lesion in the lenticular nuclei (Rev Neurol, 1988, Vol. 144:5, pp. 365-367).
Treatment with D penicillamine can induce changes in the brain. This has been described by neuropathologists in literature (Clinical Neuropathology, March 1988, Vol. 7:2, pp. 62-67); however, the MR brain imaging correlates of D penicillamine therapy and toxicity are neither yet established nor available. Therapy with penicillamine can result in abnormal glial cells or gross or microcavitary changes in the putamen, and the severity of the neuropathologic findings is directly proportional to the cerebral copper content.
One entity, particularly of concern to the radiology practice in India, is Japanese encephalitis. The MR findings of Japanese encephalitis and Wilson's disease are quite similar despite being different entities (European Radiology, April 2002, Vol. 12:4, pp. 872-876). The topographical distribution of lesions were similar, with predominant involvement of the basal ganglia and thalami, but differences on imaging included more frequent brain stem lesion and sparing of posteromedial part of the thalami in Wilson’s disease. In Japanese encephalitis, specifically hyperintense basal ganglia on T2-weighted images, subacute hemorrhage in the thalami, and meningeal enhancement were characteristically seen.
MRS is of value in differentiating changes in the brain due to copper deposition from changes due to portosystemic encephalopathy. Specifically, MRS in Wilson's disease shows decreased NAA, indicating neuronal degeneration which is a part of the neurodegeneration by the heavy metal deposition (Magnetic Resonance Imaging, January 2002, Vol. 20:1, pp. 131-135). If associated with portosystemic shunting leading to metabolic encephalopathy, myo-inositol is decreased (Radiology, May 1997, Vol. 203:2, pp. 539-543).
By Colonel M.N Sree Ram, Lt Col C.M Sreedhar, Wg Cdr A Alam, Surg Cdr I.K Indrajit and Maj Kavita Manrai, AFMC, Pune
AuntMinnieIndia.com contributing writers
August 5, 2004
Col M.N Sree Ram, MD, is Professor and Head, Department of Radiodiagnosis and Imaging, Armed Forces Medical College, Pune.
Copyright © 2004 AuntMinnie.com