Intraoperative radiotherapy (IORT) administered as a boost during breast surgery provides outstanding tumor control outcomes compared to a conventional boost, attendees were told at the European Society for Therapeutic Radiology and Oncology (ESTRO) meeting earlier this month in London.
The latest long-term results were compiled from a pooled analysis of data from members of the European group of the International Society of Intraoperative Radiation Therapy (ISIORT).
The results showed an impressively lower in-breast cancer recurrence rate of 1.6% for patients who received linac-based IORT with electrons as a boost strategy followed by whole-breast radiotherapy treatment, compared with a recurrence rate of 7.2% for patients who received a conventional boost. Dr. Felix Sedlmayer, chairman of the department of radiotherapy and radio-oncology at the University Clinic Salzburg, presented the findings.
The patient cohort included 1,110 patients who received treatment for early-stage breast cancer at one of seven hospitals through September 2005. Fifty-two percent of the patients presented with at least one adverse prognostic factor that included a large and/or high grade of tumor, nodal involvement, and/or young age. All healthcare institutions participating in the study used parallel methods, sequencing, and dosage for both intraoperative and postoperative radiotherapy treatments.
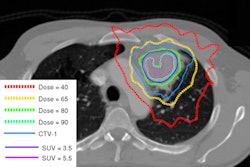
A median single fraction dose of 10 Gy was applied to the tumor bed, mainly by electron energies of 4, 6, and 8 MeV using round Perspex tubes with a 5 to 8 cm diameter. The investigators aimed to treat a target volume comprised of 3 cm in all directions calculated from the macroscopic form tumor site encompassed by 90% isodose.
Whole-breast irradiation delivering 50 to 54 Gy was performed after a median time span of 48 days. Almost all patients received additional adjuvant systemic therapy.
"We were lacking long-term data, so we invited institutions to contribute findings on mobile or fixed linacs using 52- to 54-Gy breast radiotherapy in single doses between 1.7 and 2 Gy," Sedlmayer pointed out.
The most recent analysis from data compiled through March 2009 represented a median follow-up of 73.3 months of all living patients. At this time point, 10% of patients had developed metastases, 87.8% had disease-free survival, and 93.3% had disease-specific survival.
Overall survival was 89.7%. Out of the 108 patients who had died, 57 had died from cancer and 13 from a secondary tumor.
Sedlmayer emphasized that the most important results related to what actually happened within the treated breast. "Our findings are superior to every published evidence after conventional boost treatment," he said. "We saw 16 in-breast recurrences, half of which were true local recurrences. This yields a local tumor control rate of 99.2% at 73.3 months."
A subanalysis of the data showed that a patient's age (younger than 40 years) was the most relevant factor for developing an in-breast recurrence, he added. Other predictive factors for recurrence included grade 3 tumors and negative hormonal status.
Comparing conventional boost with IORT boost
The analysis also focused on the key question of whether IORT as a boost strategy was better than a "classical" boost. To address this, 188 patients who received an external electron boost (6 x 2 Gy Dmax [1.8 Gy Dref]) were compared with 190 patients who received an IORT boost (10 Gy Dmax [9 Gy Dref]). Patients were matched by age, menopausal status, tumor size, histological type, grading, and nodal status.
Discussing the still-to-be-published 10-year comparison results, Sedlmayer said, "We see a significant difference between the in-breast recurrence rate at 10-years follow-up. All of these are almost entirely due to a reduction in true local recurrence. At 10 years, the in-breast recurrence rate is 7.2% in the external electron boost group and 1.6% in the IORT group."
The next step, which began in January 2011, is the multicenter Intraoperative Electron Boost and Hypofractionated Whole-Breast Irradiation During Breast-Conserving Treatment (HIOB) clinical trial, which is also being conducted by ISIORT. Five-year recurrence rates after the HIOB treatment will be benchmarked against the respective, best published results to date with non-IORT approaches across three age groups of patients.
Dr. Barbara Jereczek-Fossa, senior deputy director of the division of radiotherapy of the European Institute of Oncology at the University of Milan, said that the results showed outstanding local tumor control rates.
She also said that she supported the use of radiotherapy directly to the tumor bed at the time of surgery, suggesting that the availability of mobile linear accelerators may better allow administering some radiotherapy directly to the tumor bed in the operating room, followed by a short course of whole-breast radiotherapy.