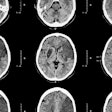
Researchers in South Korea used a dual-energy CT (DECT) scan to perform a lung imaging task that previously required two scans, reducing the radiation dose needed for the workup.
The team, from the University of Ulsan College of Medicine in Seoul and Siemens Healthcare (Erlangen, Germany), found that dual-energy CT enabled the detection of both contrast enhancement and lung nodule calcifications in a single scan.
Distinguishing benign from malignant solitary pulmonary nodules (SPN) requires careful analysis of nodule size, morphology, and CT attenuation in a challenging imaging environment where most patients present with SPN, but nearly all SPN are benign.
"Chest CT is usually performed as a combination of nonenhanced and enhanced scanning," wrote Dr. Eun Jin Chae; Dr. Jae-Woo Song, Ph.D.; Dr. Joon Beom Seo, Ph.D.; and colleagues. "A nonenhanced scan is obtained for the detection of calcification in the SPN or in the lymph node, since the presence of calcification is one of the important deterministic findings of benignity. An enhanced scan is informative in providing the degree and pattern of enhancement with use of iodine. In particular, the degree of enhancement of an SPN after iodine injection has proved to be helpful for distinguishing malignant from benign nodules" (Radiology online, September 16, 2008).
Operating the dual-source CT scanner's two x-ray tubes at two different settings enables the acquisition of dual-energy (DE) data, which in turn allows differentiation of iodine from other materials due to its stronger photoelectric absorption, the authors explained.
"One potential application of iodine differentiation with the [dual-energy] technique is to differentiate contrast material-enhanced structures from the otherwise dense material in parenchymatous organs," such as the differentiation of calcification from enhancing tissues in SPN.
The study examined 49 patients (26 men, 23 women; mean age, 60.39 years ± 12.24) with dual-source CT in DE mode. The scans were obtained before and three minutes after injection of 100 mL iomeprol contrast (Iomeron 300, Bracco, Milan, Italy) at a rate of 3.0 mL/sec with the aid of a power injector.
The dedicated DECT protocol employed tube currents of two x-ray tubes of 80 kV and 140 kV and were fixed as a ratio of approximately 4:1 (50 mAs [effective] for 80 kV and 210 mAs [effective] for 140 kV).
All scans were performed with a Somatom Definition scanner (Siemens Healthcare) using 14 x 1.2-mm collimation, 50 mAs (effective) at 140 kV and 210 mAs (effective) at 80 kV, pitch of 0.7, and rotation time of 0.5 seconds.
"Each tube has 24 rows of 1.2 mm; however, only some of them were used (14 x 1.2 mm) to allow for an improved scatter-correction by using the outer rows. The craniocaudal direction was used for all scans," they wrote.
In 25 patients who had previously undergone a conventional chest CT, SPN-targeted DECT scans were obtained before and three minutes after contrast injection. In 24 patients who had not been scanned previously, the researchers added to the first protocol a one-minute-delayed scan of the full thorax.
For all patients, the data from both tube current settings, the weighted average image of nonenhanced CT, and the targeted three-minute-delayed scans were examined on a workstation (MultiModality Workplace, Siemens Healthcare). The one-minute-delayed scans in the 24 first-time patients were examined on a PACS network.
To assess their ability to successfully differentiate the iodine component, the researchers placed two regions of interest (ROIs) manually on their "virtual nonenhanced" images (e.g., created in postprocessing from enhanced images), on nonenhanced weighted average images, and on the CT-weighted average image, Chae and colleagues explained.
"The sum of the CT number of SPN on iodine-enhanced image and virtual nonenhanced image was compared with the CT number on the enhanced weighted average image," they stated. "The CT numbers of the SPN on iodine-enhanced image and the degree of enhancement were compared in terms of their diagnostic accuracy for distinguishing malignant and benign nodules with a 20-HU threshold."
According to the results, CT values for both virtual nonenhanced and nonenhanced weighted average images and the values for iodine-enhanced image and the degree of enhancement showed good agreement (intraclass correlation coefficients of 0.83 and 0.91, respectively), the authors reported.
"Diagnostic accuracy for malignancy by using CT numbers on iodine-enhanced images was comparable to that [of] using the degree [of] enhancement (sensitivity, 92% and 72%; specificity, 70% and 70%; accuracy 82.2% and 71.1%, respectively)," they wrote.
On the virtual enhanced image, the team detected 85% (17/20) of calcifications in the SPN and 97.8% (44/45) of the lymph node calcifications. However, the sizes of the calcifications on the virtual nonenhanced images were smaller than those on the nonenhanced weighted average images in all 14 patients with calcification.
The average dose-length product (DLP) was 92.77 mGy cm ± 32.37 in protocol 1 (25 previously scanned patients) and 333.54 mGy cm ± 53.93 in protocol 2 (24 first-time patients). The average DLP for the one-minute-delayed thoracic scan in protocol 2 was 240.77 mGy cm ± 37.18.
"This was not significantly different from the average dose-length product of CT examinations performed by using single-energy multidetector CT and dual-source CT without the application of the DE mode (235.38 mGy cm ± 35.40 and 233.13 mGy cm ± 67.36, respectively) (p = 0.67 and 0.39, respectively)," they wrote.
The results showed that iodine could successfully be differentiated from enhanced soft tissue at DECT, they concluded. DECT also enabled measurement of the degree of enhancement with iodine and the detection of calcifications without additional radiation dose.
The degree of enhancement of an SPN after iodine injection has proved to be helpful for distinguishing benign from malignant nodules, a test that DECT can now perform in a single scan, and using the same ROI, they wrote. This means that the new method might reduce measurement error due to different placement of the ROI in sequential images, potentially a very important advantage when evaluating smaller nodules.
The demonstration of calcification was not comparable between the virtual nonenhanced scan and the nonenhanced weighted image, however. Most calcifications appeared smaller, most likely due to partial-volume effect. Moreover, 6.2% of the calcifications were not visualized on the virtual nonenhanced images. This may also be due to increased image noise and reduced signal-to-noise ratios in those images, they suggested.
Differentiating calcification from contrast is important, inasmuch as the presence of calcification implies benign etiology, they wrote. Their institution performs only enhanced scans due to relatively low benefit of nonenhanced scanning and the fact that it doubles the radiation dose, they noted.
However, a single scan is not an optimal solution, Chae and colleagues wrote. "Enhancement of an SPN after iodine injection often obscures the presence of calcification in the nodule, especially if the calcification does not show substantially higher attenuation than the peak level of enhancement of the nodule."
In the present study, obscured calcifications on virtual nonenhanced imaging were detected in two patients. Therefore, even if the virtual nonenhanced images turn out to be slightly less valuable than a nonenhanced scan, they are still useful "when high attenuation is equivocal on an enhanced CT image," they wrote. When this occurs, a virtual nonenhanced image can be postprocessed retrospectively for problem-solving.
Limitations of the study included the 26-cm field-of-view on the smaller DECT model used, as well as the small number of patients, the authors noted. Further studies will be needed to prove the reliability of the method for detecting calcification and measuring the degree of iodine enhancement.
By Eric Barnes
AuntMinnie.com staff writer
October 8, 2008
Related Reading
CAD detects more lung nodules but not necessarily more cancer, September 24, 2008
Modest mortality gains in CT lung screening model, July 22, 2008
Smoking during radiation therapy reduces treatment benefit, July 16, 2008
Diligence can reduce missed lung cancers in CT, June 23, 2008
Ground-glass nodule features on CT reveal malignancy risk, April 29, 2008
Copyright © 2008 AuntMinnie.com
















![Images show the pectoralis muscles of a healthy male individual who never smoked (age, 66 years; height, 178 cm; body mass index [BMI, calculated as weight in kilograms divided by height in meters squared], 28.4; number of cigarette pack-years, 0; forced expiratory volume in 1 second [FEV1], 97.6% predicted; FEV1: forced vital capacity [FVC] ratio, 0.71; pectoralis muscle area [PMA], 59.4 cm2; pectoralis muscle volume [PMV], 764 cm3) and a male individual with a smoking history and chronic obstructive pulmonary disorder (COPD) (age, 66 years; height, 178 cm; BMI, 27.5; number of cigarette pack-years, 43.2, FEV1, 48% predicted; FEV1:FVC, 0.56; PMA, 35 cm2; PMV, 480.8 cm3) from the Canadian Cohort Obstructive Lung Disease (i.e., CanCOLD) study. The CT image is shown in the axial plane. The PMV is automatically extracted using the developed deep learning model and overlayed onto the lungs for visual clarity.](https://img.auntminnie.com/mindful/smg/workspaces/default/uploads/2026/03/genkin.25LqljVF0y.jpg?auto=format%2Ccompress&crop=focalpoint&fit=crop&h=112&q=70&w=112)