Researchers have identified a biomechanical predictor of emergency caesarean section (ECS) as well as particular patterns of altered brain activity in women with postpartum post-traumatic stress disorder (PP-PTSD), according to a poster presented May 14 at the ISMRM meeting in Capetown, South Africa.
The findings could help clinicians gain a clearer picture of PP-PTSD's neurological underpinnings and develop new tools for early psychological intervention, wrote a group led by Bo Li, PhD, of the 960th Hospital of the PLA Joint Logistic Support Force in Jinan, China.
"Predicting traumatic birth events, such as [ECS], could allow timely psychological support," it wrote.
PP-PTSD affects about 20% of women around the world, and ECS is a key risk factor for it, the researchers explained, noting that birth trauma can lead to "intrusive memories, avoidance, and hyperarousal, severely affecting maternal-infant bonding and mental health." Yet the predictors and neural basis of PP-PTSD aren't clear, Li and colleagues explained.
To address the knowledge gap, the investigators conducted a study that included 245 pregnant women who planned on vaginal delivery. During the birth process, clinicians measured fetal head descending thrust at three stages of cervical dilation using internal tocodynamometry (which consists of placing a pressure-sensitive catheter directly inside the uterus, alongside the baby).
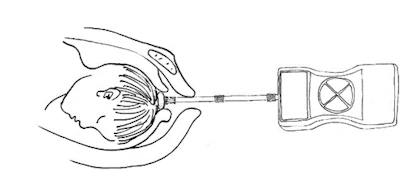 Schematic diagram of self-developed internal tocodynamometry machine.Bo Li, PhD, and ISMRM
Schematic diagram of self-developed internal tocodynamometry machine.Bo Li, PhD, and ISMRM
At one month postpartum, 26 women met diagnostic criteria for PP-PTSD based on DSM-V (Diagnostic and Statistical Manual of Mental Disorders, 5th edition) and CCMD-3 (Chinese Classification of Mental Disorders, 3rd Revision) standards. These women were matched with a control group of 28 women without PP-PTSD; all underwent 3-tesla resting-state fMRI.
Lo and colleagues analyzed labor monitoring data and reported that fetal head descending thrust values below 16.29 N at 5 cm to 8 cm dilation and below 26.36 N at 8 cm to10 cm dilation were significantly associated with higher rates of emergency caesarean section. Study data also showed an area under the receiver operating curve (AUC) of 0.896 for predictive accuracy at the 5 cm to 8 cm dilation stage, and an AUC of 0.786 at 8 cm to 10 cm dilation stage.
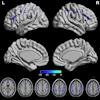
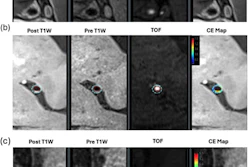
In addition to the labor monitoring data, the group analyzed study participants' resting-state fMRI results, particularly a measure of spontaneous neural activity called amplitude of low-frequency fluctuations (ALFF). It found that women with PP-PTSD had significantly reduced ALFF in the bilateral insular cortex, the right anterior cingulate cortex, and the left midcingulate cortex compared to women without the condition, and noted that these regions form "core nodes of the brain's salience network, which governs emotional processing, interoception, and cognitive control."
 The PPD group showed significant increased VMHC in the dorsolateral prefrontal cortex (DLPFC), precentral gyrus (PreCG) and parietal lobule (PL) (FDR correction q-value < 0.005).Bo Li, PhD, and ISMRM
The PPD group showed significant increased VMHC in the dorsolateral prefrontal cortex (DLPFC), precentral gyrus (PreCG) and parietal lobule (PL) (FDR correction q-value < 0.005).Bo Li, PhD, and ISMRM
The research results could translate into better postpartum care, according to the group.
"Identifying women at risk of emergency caesarean section through tocodynamometry creates a critical window for preemptive emotional support, potentially reducing the incidence of the disorder before it develops," it concluded.