The disparity in AI tools for pediatrics is tied to a lack of public pediatric medical imaging data to support their development, according to a recent study.
Across 203 public datasets reviewed, researchers found that 33% of datasets lacked metadata on patient ages, and when available, children represented less than 2% of patients.
“Despite forming a significant portion of the population, children are almost invisible in the datasets accelerating advancements in AI for medical imaging,” noted lead author Stanley Bryan Zamora Hua, PhD, of the Hospital for Sick Children in Toronto, and colleagues. The study was published April 24 in Nature Health.
AI has the potential to transform healthcare for all patients, yet there are disproportionately fewer pediatric AI studies and U.S. Food and Drug Administration (FDA) approvals relative to adults, indicating less effort focused on AI for children, according to the authors. Moreover, AI models trained on adult data cannot generalize safely to younger patients, the authors noted.
To assess the scope of the problem, the group conducted a review of 203 public medical imaging datasets drawn from major public sources and assessing each dataset for patient age metadata and quantified pediatric representation. In addition, to illustrate how a lack of pediatric data can lead to harmful algorithmic bias, the researchers trained AI models to classify adult cardiomegaly and evaluated them on healthy children in the only large-scale public pediatric chest x-ray dataset available.
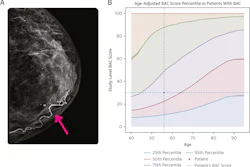
Among the 135 datasets with usable age data, children accounted for just 6,026 of 512,608 patients (under 2%), according to the analysis. Only five datasets were explicitly pediatric-only. The data gap varied significantly by modality: for every pediatric x-ray image in public datasets, there were 128 adult x-ray images; for CT the ratio was 317 to one, and for MRI the ration was 298 to one. By comparison, children account for approximately 4% of real-world imaging examinations in the U.S., suggesting that public datasets substantially underrepresent pediatric imaging relative to clinical practice, Hua and colleagues noted.
In the cardiomegaly case study, they found that AI classifiers trained on adult data showed the highest false-positive rates in children under two, with false-positive rates declining steadily as patient age increased. This pattern persisted even after adjusting for known image-contrast differences between pediatric and adult x-rays, the team reported.
“The lack of public pediatric data hinders the development of safe AI for children, producing a landscape of adult-first and adult-only AI models with unknown patterns of bias in children,” they wrote.
Ultimately, a solution to the pediatric data gap will not arise naturally, according to the authors. They called on healthcare institutions, researchers, and policymakers to prioritize pediatric data collection and release, mandate patient-level age reporting, and create dedicated pediatric AI benchmarks and challenges.
"This work not only quantifies the extent of this problem but demonstrates the potential of systematic failure on children when using AI models trained only on adults,” they concluded.
The full study is available here.



![Representative example of a 16-year-old male patient with underlying X-linked adrenoleukodystrophy. (A, B) Paired anteroposterior (AP) chest radiograph and dual-energy x-ray absorptiometry (DXA) report shows lumbar spine (L1 through L4) areal bone mineral density (BMD). The DXA report was reformatted for anonymization and improved readability. The patient had low BMD (Z score ≤ −2.0). (C) Model (chest radiography [CXR]–BMD) output shows the predicted raw BMD and Z score in comparison with the DXA reference standard, together with interpretability analyses using Shapley additive explanations (SHAP) and gradient-weighted class activation maps. The patient was classified as having low BMD, consistent with the reference standard. AM = age-matched, DEXA = dual-energy x-ray absorptiometry, RM2 = room 2, SNUH = Seoul National University Hospital, YA = young adult.](https://img.auntminnie.com/mindful/smg/workspaces/default/uploads/2026/04/ai-children-bone-density.0snnf2EJjr.jpg?auto=format%2Ccompress&fit=crop&h=167&q=70&w=250)