Deuterium metabolic imaging (DMI) can measure treatment response in high-grade glioma patients undergoing chemoradiotherapy, according to study presented May 12 at the International Society of Magnetic Resonance in Medicine (ISMRM) meeting.
The findings is from a prospective two-site study in which 18 patients with newly diagnosed high-grade glioma underwent DMI, with the technique further demonstrating that pre-treatment metabolic ratios may predict progression-free survival, noted presenter Alixander Khan, PhD, of Aarhus University in Denmark.
“Early assessment of high-grade glioma treatment response is confounded by pseudoprogression on conventional MRI, highlighting the need for more specific noninvasive metabolic biomarkers,” Khan noted.
Deuterium is a stable, nontoxic isotope used to label glucose, which is then administered as an oral imaging agent. Tumor cells take up and metabolize the labeled glucose, with MRI scans then able to detect the deuterium signal and map the tumor's downstream glucose metabolism. Preclinical studies have shown the technique can offer a marker of tumor aggressiveness, the authors noted.
To further assess the technique, Khan and colleagues recruited 18 patients with newly diagnosed high-grade glioma at Aarhus University Hospital and Cambridge University Hospital. All but one patient were IDH wildtype and all had undergone surgery prior to baseline scanning. Patients fasted for a minimum of four hours before receiving oral imaging agent.
After imaging on clinical 3T MRI systems, the team calculated glycolytic (Lac/Gluc) and oxidative (Glx/Gluc) metabolic ratios, normalized longitudinal changes to the contralateral normal-appearing brain parenchyma (NABP), and analyzed progression-free survival (PFS) and overall survival (OS).
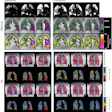
 Representative DMI data from a patient with a high-grade glioma. DMI ratio maps pre- and post-treatment show spatial metabolic changes. Deuterium spectra from the tumor and contralateral NABP demonstrate metabolic differences and therapeutic effects. Alixander Khan, PhD, and ISMRM
Representative DMI data from a patient with a high-grade glioma. DMI ratio maps pre- and post-treatment show spatial metabolic changes. Deuterium spectra from the tumor and contralateral NABP demonstrate metabolic differences and therapeutic effects. Alixander Khan, PhD, and ISMRM
In contrast, the longitudinal change in the Glx/Gluc ratio was heterogeneous across the patient cohort. A Kaplan-Meier survival analysis revealed that a lower pre-treatment normalized Glx/Gluc ratio within the tumor was a significant predictor of shorter PFS (median PFS: 98 days for the below-median group vs. 351 days for the above-median group; p = 0.034). Lastly, Glx/Gluc within the contrast enhancing region also showed a strong trend towards predicting poorer OS (p = 0.0599), according to the findings.
“DMI is a promising, noninvasive imaging tool that provides biologically relevant information for assessing treatment response in high-grade glioma,” the group wrote.
Ultimately, reliable early response evaluation is vital to guide treatment decisions and avoid continuing ineffective therapies in patients with high-grade glioma, which carries a median survival time of 15 months and a five-year survival rate of 5% to 10%, Khan noted. In this regard, DMI shows promise and warrants further investigation.
"The ability to measure a longitudinal decrease in glycolysis (Lac/Gluc) offers a potential method for assessing treatment efficacy earlier than is possible with standard anatomical imaging," Khan and colleagues concluded.
Check out AuntMinnie's full coverage of ISMRM 2026 on our ShowCast.