A new report from the U.S. Government Accountability Office (GAO) takes a hard line on physician self-referral of imaging services, detailing more than $100 million in annual unnecessary spending in CT and MRI alone. The report recommends steps to curb the practice, including a pay cut for self-referred imaging studies.
Physician self-referral of patients to imaging scanners that they purchase or lease is a hotly contested topic. The practice is allowed through a loophole in the Stark anti-self-referral act, and proponents claim it offers convenience to patients who don't have to be referred to another facility for imaging exams.
Opponents, however, believe it leads to wasteful spending as nonradiologist physicians order imaging exams for economic rather than clinical reasons. Radiology advocates have long requested that the U.S. government address physician self-referral as part of its efforts to control wasteful healthcare spending.
The GAO report is a sign that the government may be listening. The report was commissioned due to concerns over Medicare Part B expenditures -- including those for advanced imaging services -- which "are expected to continue growing at an unsustainable rate," according to the report. The GAO said it was asked to examine the prevalence of imaging self-referral and its impact on Medicare spending.
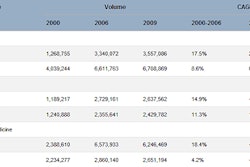
The GAO report analyzed Part B claims data from 2004 through 2010, specifically focusing on CT and MRI services. The report found that the overall incidence of self-referral grew during the period, with the number of self-referred MRI studies increasing by 80% over the study period, compared to growth of 12% for MRI scans that weren't self-referred.
In addition, healthcare providers who began to self-refer saw imaging volume spike shortly after they began the practice. Providers who began self-referring in 2009 increased their CT and MRI referrals by 67.3% in 2010 compared to 2008, and the average number of referrals increased from 25.1 to 42.0 during those years.
In comparison, physicians who were already self-referring in 2009 saw their imaging volumes drop 3.4%, from an average of 47.0 referrals in 2008 to an average of 45.4 referrals in 2010. For providers who weren't self-referring at all, imaging volumes fell 6.8%, from 20.6 referrals in 2008 to 19.2 in 2010. The findings suggest that the increase was not due to an overall rise among all providers, according to the GAO.
The report estimates that in 2010, healthcare providers who self-referred likely made 400,000 more referrals for advanced imaging studies than they would have if they were not self-referring, and these referrals probably cost Medicare $109 million. The referrals are particularly problematic for CT, as they are exposing patients unnecessarily to ionizing radiation.
The report makes several recommendations to help the U.S. Centers for Medicare and Medicaid Services (CMS) identify and rein in self-referred imaging studies:
- The CMS administrator should insert a flag to identify self-referred imaging studies on Medicare Part B claims forms. Providers should be required to indicate whether the services for which they are billing are self-referred.
- CMS should implement a payment reduction for self-referred advanced imaging studies to recognize the efficiencies that occur when the same provider refers and performs a service.
- CMS should develop tools for ensuring the appropriateness of self-referred imaging services.
Response to the report was mixed. The Medical Imaging and Technology Alliance (MITA), which represents scanner vendors, found fault with the report, stating that two of the recommendations were "unworkable and unnecessary." The report also failed to acknowledge that per capita imaging utilization has declined, and it failed to address patient access to imaging.
MITA believes that qualified physicians should be able to provide appropriate imaging services to their physicians regardless of their specialties -- to do otherwise would limit patient access to care. MITA also noted that the U.S. Department of Health and Human Services (HHS) has agreed to examine the appropriateness issue, which MITA believes is best tackled through appropriateness criteria developed by physicians.