Technetium Labeled Cardiac Imaging
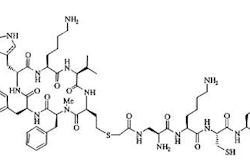
Tc-99m-Sestamibi (2-methoxyisobutyl-nitrate) and Tc-99m-Tetrofosmin
Advantages
Technetium agents have the following advantages when compared to thallium:
1- Energy: The 140keV photon is optimal for gamma camera imaging and can produce higher quality images due to less attenuation, less scatter, and a brighter flash within the scintillation detector (Thallium uses low energy Mercury photons [60-83keV] which have high tissue attenuation).
2- Shorter half-life: Technetium has a 6 hour half-life, as opposed to 73 hours for Tl-201. Therefore, one can administer a 10 to 15 times higher dose than thallium which results in a higher count rate [47]. With the use of a larger dose, images can be obtained in a shorter period of time. High count rates also permit the use of gating to assess wall motion and ejection fraction [47].
3- Production: Technetium is available via a generator 24 hours a day. Thallium is cyclotron generated and requires off-site delivery.
Physiology & Pharmacology
Tc-Sestamibi:
Sestamibi is a lipophilic monovalent cation (an isonitrile compound) [104]. It enters the cell via passive diffusion across plasma and mitochondrial membranes. It is postulated that MIBI accumulates within the mitochondria and cytoplasm of cells on the basis of electrical potentials generated across the membrane bilayers. At equilibrium it is sequestered largely within mitochondria (90%) by a large negative transmembrane potential. The agent is unmetabolized [11] and is fixed intracelluIarly as long as cell membrane integrity is intact and nutrient blood flow persists. It will not be extracted by non-viable myocardium. In plasma, less than 1% of the tracer is protein bound. Prior to use, the radiochemical purity of Tc-Sestamibi should be greater than 90%. Ethanol is the solvent used for quality controlusing paper chromatography. Sestamibi migrates to the top of the strip. Adverse reactions to Sestamibi are rare (less than 0.5%) and there have only been a couple of case reports of anaphylaxis [105].
The first pass extraction fraction for Tc-Sestamibi is approximately 65% (lower than that for thallium, which has an extraction fraction of about 85%) [47]. About 1-2% of the injected dose localizes to the myocardium at rest. The lower extraction fraction is overcome by the larger dose of MIBI which results in a higher count rate. Additionally, after initial extraction, blood levels fall rapidly which provides excellent target to background ratios as long as liver and bowel do not interfere with the image.
The uptake of Sestamibi in the myocardium is proportional to blood flow in the physiologic flow range. However, there is a plateau in extraction at higher flow rates, most likely because the tracer enters the cell via diffusion [22,47]. This plateau in extraction occurs at a lower level of increased flow above baseline compared to Tl-201 [47]. Because of the extraction plateau, Tc-sestamibi will underestimate blood flow at high flow rates (>2.0mL/min. per gram or about 2.5-3 times baseline flow [22,47]). Such high flow rates are encountered when using pharmacologic stress agents such as dipyridamole or adenosine. Therefore, it is theoretically possible for a mild to moderate stenosis which does not significantly impair coronary artery flow reserve to be overlooked with sestamibi vasodilator stress imaging [22]. Even so, the higher spatial resolution and lack of redistribution may offset the expected finding of slightly lower defect contrast associated with this reduced extraction at higher flow rates when compared to thallium. Overall, Tc-sestamibi is primarily a perfusion agent- it provides only limited information regarding myocardial viability and will frequently overestimate the amount of myocardial scarring.
Myocardial clearance of Tc-sestamibi is slow and the agent does not redistribute to a degree that can be imaged clinically [16]. Note (the following is certainly beyond what would ever be expected of a radiology resident): Heart House Course, Bethesda '93: Sestamibi undergoes minimal (about 20%) redistribution primarily within the first 20 to 60 minutes following injection. This may impact on lesion detection as the differential washout between the normal and ischemic myocardium may result in a reduction in defect size or severity with time. Therefore, their recommendation was to begin imaging 15 minutes following stress injection, and 60 minutes following rest injection. The tracer is retained in normal myocardium for several hours (myocardial clearance T1/2 is about 5 hours). Myocardial washout of MIBI is increased in patients with chronic heart failure [104] and an area of reverse-redistribution can be seen following PTCA in patients with acute MI- indicating that the ability of myocytes to retain the tracer may be impaired in stunned myocardium (possibly related to loss of the normal membrane potential or mitochrondrial injury) [84].
The primary route of excretion is hepatobiliary (33%). Clearance via this route is prompt (T1/2 of approximately 30 min.). Unfortunately, scatter from both liver and bowel activity can interference with visualization of the inferior ventricular wall. This activity can be backprojected over the inferior wall during image reconstruction. High hepatic uptake can also create artifactual perfusion defects in the inferior and inferoseptal walls [1]. Finally, this activity may also severely disrupt image normalization programs. There is about 25% renal clearance of the agent. The critical organ is the upper large intestine, which receives about 5.4 rads per 30mCi dose of Sestamibi. Total body dose is about 500mrem to 1.2 rem (12 mSv) for a 1 day rest-stress exam using 10mCi + 30 mCi [78].
Tc-MIBI does not concentrate in breast milk to any significant degree and cessation of breast feeding is not necessary following a Tc-MIBI exam. Close contact with the infant, however, should be avoided [17].
Technetium-99m-Tetrofosmin [1,2-bis [bis (2-ethoxyethyl) phosphino] ethane]
Tetrofosmin is a lipophilic, cationic, diphosphine which is rapidly cleared from the blood following intravenous administration [47]. The agent requires only a 15 minute incubation at room temperature for preparation. The agent is taken up by the heart, skeletal muscle, liver, spleen, and kidneys in proportion to blood flow and viability [24]. Between 1 to 1.5% of the injected dose localizes to the myocardium. The uptake mechanism is membrane-potential driven diffusion independent of cation channel transport [24]. The agent accumulates within mitochondria similar to Tc-sestamibi [47]. Myocardial uptake is decreased by metabolic inhibitors that cause severe cell injury or cell death [47].
The agent does not redistribute to any significant degree, but the higher lipophilicity may explain its higher initial uptake and faster washout [24]. The biological half-life for tetrofosmin in normal myocardium is 278 +/- 32 minutes, which is shorter than sestamibi (680 +/- 45 minutes) [24]. Hepatic uptake is lower than with Tc-Sestamibi and it also clears more quickly which can permit imaging sooner after injection (as soon as 5-15 minutes after exercise injection and 30 minutes for rest injection) [19,20,24,111].
The mean first pass extraction fraction is about 54% [47]. As with Tc-Sestamibi there is decreased tracer extraction compared to Thallium at high flow rates (such as that encountered with pharmacologic stress). The extraction of Tetrofosmin plateaus at a flow rate of approximately 2.0 mL/min/gm3 (or about 1.5 times normal flow [47]). The heart to lung contrast ratio is similar to sestamibi between 30 to 60 minutes post-injection [24]. Similar to Tc-Sestamibi, lesion conspicuity for mild to moderate stenoses may be less apparent than for Tl201 [47]. The typical total-body effective dose from a one day rest-stress exam using 10 mCi + 30 mCi is about 1.06 rem (10.6 mSv) [78]. Adjustments to the amount of radiotracer used can be made based upon patient size (i.e.: increase the doses to 15 mCi + 45 mCi for patients over 300 lbs) [85]. Patients over 350 pounds should undergo a two-day protocol [85].
Sensitivity & Specificity
The sensitivity/specificity for SPECT Tc-Sestamibi and Tc-Tetrofosmin in the detection of coronary artery disease are almost identical to thallium (sensitivity of about 90% and specificity of about 80%) [2].
Perfusion imaging of female patients poses certain challenges- specifically women have a relatively smaller heart size, there is attenuation associated with breast tissue, and they have a lower prevalence of CAD [88]. The reported overall accuracy for technetium agent perfusion imaging in women is sensitivity 71-83%, specificity 80-86%, and accuracy 82% (with higher sensitivity for multi-vessel compared to single vessel disease and for higher grade stenoses) [89].
The use of attenuation correction can improve the specificity, normalcy, and accuracy of the perfusion exam [53,54,68,75,101]. Radioisotope-based attenuation correction requires sources that must be replaced as they decay [101]. Attenuation correction can also be accomplished with hybrid SPECT systems that utilize CT [69,75,101]. CT attenuation correction has been shown to improve the diagnostic yield of SPECT imaging for detecting significant CAD (greater than 50% stenosis) [75]. However, misalignment between the transmission and emission studies can be a major source of artifacts [97] and misalignment can be found in up to 42% of studies [98,103]. Despite this misregistration, the exam results may not be significantly affected [103] However, a careful review of image registration should be performed to avoid reconstruction artifacts due to misregistration [103]. A slow CT acquisition with a 4 second rotation during free breathing may provide better image registration between the SPECT and CT data sets [73]. Severe CT related artifacts (from beam hardening) can render up to 8% of studies uninterpretable [103]. One added benefit of using CT for attenuation correction is that potentially significant abnormal findings can be found in up to 10.5% of patients on the non-diagnostic CT portion of the exam [87].
Same day Rest and Stress study
An initial rest exam followed by the stress study was found to be more effective for determining the presence of reversible abnormalities [3]. A stress/rest sequence results in an increased number of ischemic segments incorrectly being identified as fixed defects (7% false-negatives) [4]. Additionally, in the stress-rest protocol, the rest portion of the exam may not be considered to be a "true" rest study as it follows a period of exercise and this may contribute to the overestimation of scar.
Patients should fast for 4 to 6 hours prior to the exam in order to decrease heptic and GI activity [85]. The first injection (rest study) is low dose (8mCi), while the second or stress injection is high dose (22mCi- approximately 3 times the rest dose in order to overwhelm activity remaining in the myocardium) and follows the first by 2-3 hours to permit time for some decay of the agent. Rest images are obtained 1 hour after injection. Some centers have the patients drink 8oz. of whole milk about 15 minutes prior to imaging to promote tracer clearance from the liver and gallbladder. This, however, increases the amount of bowel activity.
Drawbacks of the same day rest-stress protocol are that it provides less than ideal stress defect contrast due to resting background activity. Tc-Sestamibi and Tc-tetrofosmin rest imaging have also been shown to underestimate the extent of viable tissue.
Two-day Stress/Rest Protocol
The 2 day exam provides optimal defect contrast with minimal background activity. Additionally, the rest study would not be necessary if stress study was normal.
Dual Isotope Scanning
In this protocol a rest thallium study (2.5-3.5 mCi) is done first so that there is no interference from scattered technetium photons. If Thallium is injected the day before, images will refect 24 hour redistribution (myocardial viability). Delayed thallium imaging at 24 hours using the dual isotope exam will detect reversible defects in an additional 17% of patients. [5]
A stress Tc-Sestamibi or Tc-Tetrofosmin study is then performed using 20-30 mCi of the agent. No wait is required between the rest and stress study as the Technetium gamma energy is higher than the energy imaged for Thallium. A drawback of this technique is that because of the resolution differences between the two isotopes, it is difficult to directly compare the images, particularly with subtle abnormalities.
Quantitative analysis:
A polar map is available for quantitative analysis of the images. The distance weighted map is best for determining defect location as every ring in the polar map is the same width. The volume weighted map is best for determining defect size (extent and severity), as it makes the 2-dimensional area of a defect equal to its relative 3-dimensional volume.
The summed stress score (SSS) is a commonly used technique that combines extent and severity of perfusion abnormalities (defined from a sex-specific normal database) into a single measure and it has been shown to provide risk stratificaiton [64]. Post stress and and rest perfusion images are scored using a 20 segment, 5-point model (0= normal; 1= mildly reduced uptake; 2= moderately reduced uptake; 3= severely reduced uptake; 4=absent uptake) [58]. Segmental uptake scores can then be added to produce a summed stress (SSS) and rest scores (SRS). The summed difference score (SDS) represents the difference between the SSS and SRS [58]. A segmental defect is considered fixed if the uptake score remains fixed between the stress and rest exams, mildly reversible if it increases by 1 point, moderately reversible if increases by 2 points, and severely reversible if it increases by 3 points [58]. A SDS score of less than 2 is considered normal with no evidence of ischemia [64]. A SDS of 4 to 7 indicates mild-to-moderate reversibility and a score of greater than 7 to 8 indicates severe reversibility [58]. The SRS can also provide prognostic information [102]. Patients with normal LVEF's, but a SRS of greater than 6 have a poor prognosis (2 fold decrease in survival rate) similar to patients with a reduced LVEF (less than 45%) [102].
Gating- Wall motion and LVEF assessment
In non-gated SPECT imaging one projection image is acquired at each angular step along the acquisition orbit [82]. With gated SPECT, data acquired during each angular step is further subdivided into a specific phase of the cardiac cycle (typically 8 or 16 phases) based upon the R-R interval [82]. 16 phase data sets are required for diastolic function assessment, but can suffer from low counts [82]. Summing the data from the individual phases will produce a standard SPECT image [82]. However, ventricular function data can also be assessed by review of the gated data set. Gated imaging data can add important independent and incremental prognostic information to the data obtained from the perfusion exam [52,74].
Wall motion analysis:
Gated studies can be used to assess regional wall motion and left ventricular ejection fraction when viewed in a cine display. Gated exams improve the diagnostic accuracy and specificity [57] of SPECT imaging by detecting artifacts secondary to soft tissue attenuation. The gated LVEF also provides information regarding myocardial systolic function and prognosis. Post exercise wall motion abnormalities add significant incremental value over stress myocardial perfusion alone for the identification of severe CAD [57]. Both wall motion and wall thickening should be analyzed on gated imaging. Wall motion is scored with a 6-point system: 0- normal; 1- mild (equivocal) hypokinesis; 2- moderate hypokinesis; 3- severe hypokinesis; 4- akinesis; and 5- dyskinesis [82]. Wall thickening is scored with a 4 point system from 0 (normal) to 3 (absent) [82].
The study requires performing a gated acquisition during each of the planar projections. Optimally ECG gating is performed using eight to 16 frames for the cardiac cycle. The images obtained for interpretation are sharper than non-gated images and can sometimes increase conspicuity of a perfusion defect. Both wall motion and wall thickening can be evaluated on gated cardiac exams. However, changes in heart rate can result in temporal blurring- in other words- mixing of counts from adjacent frames [51]. To minimize temporal blurring, a beat rejection window is set by specifying the acceptable deviation of each R-R interval from the expected value (a 20% window has historically been applied) [51]. Wall motion is evaluated by measuring the excursion of the ventricular endocardial surface, while wall thickening is evaluated by assessing changes in regional myocardial counts [34]. On gated images wall thickening appears as an increase in myocardial intensity (brightness) from diastole to systole. "Flashing" on review of the projection images from a gated SPECT exam is indicative of rejected beats (generally due to arrhythmias or changes in heart rate during image acquisition) which results in variation in count density in the projection images [96]. The can produce streak artifacts in the tomographic images [96].
If a perfusion defect is present on stress images and the associated wall is seen to thicken (ie: brighten) during systole, one can predict that this represents an area containing viable myocardial tissue. If no thickening is observed, the finding may represent an area of infarction (scar), however, one cannot completely exclude the presence of viable myocardium (hibernating myocardium). If there is insufficient counts from the area of the defect, viable myocardium may not be properly identified even on a gated exam. Hence, areas of hibernating myocardium may be akinetic or dyskinetic with no evidence of thickening, but will recover function following revascularization. False positive gated exams for infarction have also been described in patients with cardiomyopathies and in valvular heart disease in which non-ischemic perfusion defects and wall motion abnormalities may be seen [13].
Gated SPECT during the first hour after exercise is able to assess post-stress cardiac function [26]. Reversible perfusion defects may display post-stress stunning (transient myocardial contractile dysfunction/wall motion abnormality) in areas of ischemia [26]. The incidence and magnitude of regional wall motion abnormalities are related to the severity of ischemia [39]. The time course for resolution of ischemic post-stress wall motion abnormalities can range from immediate to up to 2 hours [32].
In patients with multivessel coronary artery disease, the degree of ischemia can be underestimated because of a relatively balanced global left ventricular hypoperfusion resulting in a normal appearing scan [32]. Post-stress regional wall motion abnormalities detected on the gated exam may be the only indicator of severe and extensive coronary disease and provides incremental diagnostic information over perfusion alone [26]. Wall motion abnormalities identified on gated SPECT imaging provide additional prognostic information [112]. Reversible wall motion abnormalities between stress and rest images are indicative of severe coronary artery disease and have been shown to be a powerful predictor of future cardiac events [65]. Patients with abnormal wall motion on gated SPECT images have an annual event rate up to 6.1%, compared to 1.6% for patients with normal wall motion [52]. Even in patients with preserved ejection fraction, the presence of wall motion abnormalities has been found to be associated with an increased risk for cardiac death (increased to 1.6% from 0.5% if no regional wall motion abnormality was identified) [112]. The cardiac death rate increased to 2.2% when the exam also demonstrated evidence of ischemia [112].
Breast attenuation, diaphragmatic attenuation, and apical thinning can all produce fixed perfusion abnormalities. On gated images, these defects will generally demonstrate normal wall thickening which would not be identified in an area of scarring. Another technical limitation of gated imaging is overestimation of viable myocardium. Approximately 5% of myocardial infarctions are seen to thicken during systole on gated images. This may occur because a small infarct is "pulled in" by adjacent normal myocardium, or the MI may be non-transmural. False positive gated exams for infarction have been described in patients with cardiomyopathies or valvular heart disease in which non-ischemic perfusion defects and wall motion abnormalities may be seen [13].
Abnormal reduced septal motion with normal wall thickening is a common finding on gated SPECT images after coronary artery bypass surgery [34,82]. This finding is felt to be related to exaggerated systolic anteromedial cardiac translation [34]. As a result of this translocation, lateral wall function is often overestimated [34]. The exaggerated cardiac mobility is thought to be related to sternotomy and pericardiotomy [34]. Discordant septal thickening with abnormal wall motion can also be seen in patients with LBBB [82].
Ejection fraction:
The cardiac ejection fraction can be calculated from the gated SPECT data and provides incremental prognostic information for risk stratification. There are several software programs which can generate the EF and all have roughly between 70-85% correlation with gated blood pool imaging determined ejection fractions [23]. With serial measurements the calculated LVEF is very reproducible [43] and has a mean variability of about 5% (+/- 3.5%) (higher variability is associated with low count examinations) [38,95]. The LVEF also has good correlation with cine MR determined values [71]. In patients with stress induced ischemia, left ventricular function may be temporarily impaired (stunned myocardium) [43,61]. Global LVEF is generally not impaired until at least 25% of the LV myocardium is ischemic [39,65]. Global LVEF impairment is also more commonly associated with anterior (LAD) ischemia [39]. Gated SPECT imaging started soon after exercise is likely more sensitive to the detection of post-stress stunning than conventional delayed imaging- particularly in patients with single-vessel disease [61,107]. In patients with "balanced" multivessel ischemia perfusion images alone may significantly underestimate the extent of CAD and an abnormal post-stress LVEF may be the only indication of underlying CAD [51,82]. A greater than 5% decrease in LVEF is an indicator of multi-vessel CAD [100]. Myocardial stunning with decreased LVEF and wall abnormalities can also be seen on gated images following both adenosine and dipyridamole stress and is also an indicator of severe CAD [80,81].
The presence of ischemia on SPECT imaging places the patient at increased risk for subsequent ischemic event, but does not correlate with survival [94]. For prognostic information regarding survival, the post-stress ejection fraction is an important determinant for the risk of cardiac death [14,82,93]. Patients with a post-stress ejection fraction of less than 30% are at an increased risk for cardiac death, regardless of the amount of ischemia identified [14]. Other authors indicate that a post-stress ejection fraction of less than 45% is associated with an elevated risk of major adverse cardiac events [49,51,57]. A greater than 5% decrease in LVEF between rest and stress has been shown to be an independent predictor for the need for early revascularization [65]. However, ejection fraction alone is not the sole determinant of the potential benefit of revascularization [93]. Although patients with ischemia benefit from revasularization (with increasing survival benefit with increasing amounts of ischemia), the combination of ischemia AND a decreased ejection fraction indicates patients that will benefit the most from revascularization [93]. This data has significant implications regarding the management of CAD patients- particularly given recent data that suggests percutaneous coronary intervention does not decrease the rate of myocardial infaction or mortality other than in the acute coronary syndrome setting [93]. In fact, patients with drug eluting stents are at risk for acute thrombosis with an incidence up to 1.3% at 9 months and a 45% case fatality rate [93].
Following myocardial infarct: In the early phases following acute MI, left ventricular dysfunction is an independent factor for risk stratification [36]. In the post-MI period, a gated LVEF of less than 40% has been associated with an increased risk for subsequent cardiac event [33]. Generally, the relative risk of death or non-fatal MI doubles for every 10% decrease in LVEF [50].
Unfortunately, early post MI left ventricular function may be impaired [36]. Dysfunctional, but viable, stunned myocardium will gradually return to normal function, and hibernating myocardium will demonstrate improve function following revascularization [36]. Assessment for contractile reserve in areas of hibernating myocardium can be performed using low dose dobutamine (LDD) echocardiography or LDD SPECT imaging (see discussion in Pharmocologic stress imaging section). In patients with dilated cardiomyopathy, an increase in SPECT LVEF following low dose dobutamine infusion can be used to predict improvement in cardiac function and heart failure symptoms after institution of beta-blocker therapy [59].
Proper ECG triggering is crucial for accurate LVEF determination- there should be a regular cardiac sinus rhythm and exclusive R-wave detection [66]. Gating errors can affect wall motion analysis and LVEF determination [46]. In patients with arrhythmias, EF fluctuations and wall thickening discordance may occur [51].The mixing of R- and T-wave triggered beats leads to a fall in the calculated LVEF [66]. With very tall T waves, the R-T phase (systole) and the T-R phase (predominantly diastole) are regarded as two cardiac cycles [46]. When the time-volume curve is generated by summation of these phases- which produces essentially a flat line [46]. Repositioning the ECG leads to increase the amplitude of the R wave and decrease the T wave can correct this error [46]. Patient motion can also affect the calculated LVEF [66]. Even one pixel of displacement can result in a change in an absolute change in LVEF of 5% +/- 4% [66].
A limitation of software for gated SPECT is overestimation of LVEF [37] and underestimation of LV end-systolic volumes in small ventricles, especially in patients with hyperdynamic LV function (the small heart error). The inaccuracy in measurements is a result of the low spatial resolution (about 15mm) of SPECT imaging which limits effective delineation of the endocardial surface used for LVEF determination [37,51]. This is particularly a problem at end-systole because the LV is at its smallest and the endocardial edges are at their closest points [23]. In fact, the endocardial edges may appear to overlap [23]. Incorrect determination of the position of the edge of the endocardial surface results in an underestimation of end-systolic volume, which results in an overestimation of the LVEF [23]. End-diastolic volume is also markedly underestimated when less than 37 mL [23]. Programs which do not rely on edge detection may provide more accurate LVEF determinations for patients with small ventricles [23]. Arrhythmias do not seem to significantly affect ejection fraction or ventricular volume determinations [25], although other authors state that LVEF determination can be affected by arrhythmias [51]- specifically a falsely low ejection fraction [96].
Ventricular volumes:
Using gated SPECT software the left ventricular end diastolic volume (normal less than 120 mL) can also be calculated and is generally within 15% of the actual end-diastolic volume when the volume is greater than 74 mL [23].
Progressive enlargement or remodeling of the left ventricle can develop during the first months after an acute MI and this has a negative influence on long-term prognosis [60]. End-systolic LV volume is an important predictive factor of long-term prognosis in patients with ischemic heart disease [60]. An end-systolic volume of greater than 70 mL places patients in a high risk category [57]. An increase in ESV of greater than 5 mL between stress and rest is also an indicator of multi-vessel CAD [100].
The presence of an increased end-diastolic volume also carries additional prognostic information. LV enlargement significantly increases the mortality rate in patients with acute MI- particularly when there is coexisting myocardial dysfunction [50]. Patients with an LVEF lower than 40% in whom LV expansion develops, have a significantly higher mortality rate compared with those who do not [50]. An increase in EDV of greater than 5 mL between stress and rest is also an indicator of multi-vessel CAD [100].
Exercise First-pass LVEF
Technetium agent first pass LVEF determination requires the use of a multicrystal camera. In patients with multivessel disease (particularly 3 vessel disease), the perfusion study may underestimate the severity coronary artery disease (balanced ischemia). These patients, however, often demonstrate a significant drop in LVEF with exercise. A normal exercise LVEF does not exclude the presence of CAD, but it is associated with a better prognosis in patients with CAD. Patients with an abnormal exercise LVEF and known CAD may benefit more from surgical intervention (CABG,PTCA) than from continued medical therapy.
First pass LVEF seems to be the single most important predictor for the risk of cardiac events in patients with known coronary artery disease. An exercise LVEF of 20-40% is associated with a 15% one year cardiac mortality rate, while an exercise LVEF < 20% is associated with a 50% one year cardiac mortality rate.Determination of first pass LVEF in association with pharmacologic stress has not been shown to add clinical information to the perfusion exam [6].
Chamber dilatation with stress
The TID ratio is calculated as the ratio of the ungated LV cavity volume after stress and at rest [82]. As with thallium imaging, transient LV dilatation is a marker of severe and extensive coronary artery disease [70]. With technetium agents, stress imaging is delayed 30 to 60 minutes following completion of stress and therefore the left ventricle (LV) is unlikely to still be transiently dilated due to ischemia. If post-stress left ventricular chamber dilatation is noted, it is most likely a reflection of diffuse subendocardial ischemia and multivessel coronary artery disease, rather than true cavity dilatation [70]. Temporary systolic dysfunction may also contribute to the apparent increased cavity size [76]. Left ventricular chamber dilatation may also be noted with pharmacologic stress and is associated with an increased risk for subsequent cardiac event (11% versus 2%) [10,72]. This most likely represents subendocardial ischemia or diffuse reduced subendocardial flow reserve [72]. The cutoff values for abnormal transient ischemic dilatation vary throughout the literature [76,82]. When comparing exercise stress technetium images to rest either rest technetium agent or thallium images, a TID ratio of greater than 1.22 is considered abnormal [58,63,72]. For adenosine stress dual-isotope imaging a TID ratio of greater than 1.36 is associated with a high sensitivity and specificity for severe and extensive CAD (sensitivity 71%, specificity 86%) [63]. The TID ratio may need to be adjusted for gender with one study suggesting an upper limit of normal for females as 1.31 and 1.18 for males [83]. A hypertensive response to exercise (BP systolic greater than 210 [men] or 190 [women]) has been reported to have a higher association with TID- even without other significant perfusion defects [110]. Although followup cath data was not available to consistently exclude the possibility of underlying CAD [110].
A planar LAO image immediately following exercise can be performed to assess true chamber size. If LV dilatation is present, there is a high association with multivessel CAD and high grade stenoses.
|
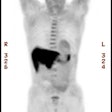
Multivessel coronary artery disease: The patient below underwent Tc-myoview SPECT imaging following pharmacologic stress with adenosine. The examination demonstrated a mild fixed perfusion abnormality in the inferolateral wall that was felt to be related to diaphragm attenuation. However, there was mild dilatation of the LV on stress imaging compared to the rest exam. At cardiac catheterization, the patient was shown to have three vessel disease. (Click image to view all slices) |
|
|
Pulmonary activity on stress imaging
An increase in Tc-sestamibi lung uptake on stress imaging is a marker for severe underlying coronary artery disease or high grade stenosis (over 90%) of the proximal LAD [29,109]. A lung to heart ratio (LHR) of greater than 0.33 has been reported as suggestive of underlying severe CAD [29]. On early sestamibi SPECT images acquired early (15 minutes) after exercise, other authors report a LHR of greater than 0.44 to yield a sensitivity of 63%, and a specificity of 81% in identifying severe and extensive CAD [109]. Diffuse lung uptake can also be seen in smokers and in patients with inhalational pneumonitis [86].
Right ventricular increased uptake:
The criterion for increased right ventricular tracer uptake on stress images is an exercise right ventricular-left ventricular uptake ratio greater than 0.42 (normal is 0.24-0.36) or exercise right ventricular-rest right ventricular uptake ratio greater than 1.2 (i.e.: a greater than 20% increase from rest to exercise) [91]. Increased right ventricular activity can be seen in conditions which produce right ventricular hypertrophy such as COPD, pulmonary arterial hypertension, and congenital heart disease (atrial septal defect) [91]. In general, these patients will have increased uptake on both stress and rest images [91]. Increased right ventricular activity on stress imaging only is sensitive (90-93%), but not specific (30-49%) for severe left main or multivessel CAD [91]. In these cases, the etiology is likely related to a global reduction in LV uptake due to hypoperfusion with relative preservation of RV tracer uptake, as well as an increase in RV wall stress associated with LV ischemic dysfunction [91].
Prognostic Value:
Risk stratification and prognostic assessment for the two agents is comparable [55].
Patients with acute chest pain
In the evaluation of patients with chest pain of suspected cardiac origin, but no ECG evidence of cardiac ischemia, Tc-Sestamibi and Tc-Myoview rest imaging can provide diagnostic and prognostic information [18,27]. Perfusion imaging in the acute setting is most useful in those patients with no history of prior MI or underlying cardiac disease [48]. The exam is less useful in patients with a history of prior MI in whom perfusion defects can be anticipated [18].
Patients injected in the ER, with evidence of a perfusion defect on the MIBI scan have a high likelihood for coronary artery disease or a myocardial infarction [9,56]. The size of the defect carries clinical implications as patients with larger defects have a worse long-term prognosis [56]. Patients with chest pain and a normal rest perfusion exam have a low likelihood for coronary artery disease and very low (less than 1%) 30 day cardiac event rate (the one-year event rate is also low - 3%) [9,56]. Based upon this data, patients could be risk stratified regarding their risk for actual cardiac event and potentially discharged [10]. Using a normal myocardial perfusion exam as a criterion NOT to admit patients can reduce total admissions and result in substantial cost savings (a 32% reduction in the odds of being admitted to the hospital to rule out MI) [27,35,92].
Additional investigators have also studied the effect of troponin levels in conjunction with MPS findings [99]. Low level elevations in cardiac troponin levels have been shown to identify patients at increased risk for future cardiovascular events [99]. However, when found to have normal MPS exams, these patients were shown to have a high-event free survival rate; whereas, an abnormal exam was associated with a 3-fold higher risk of all cause mortality and a 7-fold higher risk for 6 month cardiac events [99].
Tc-Myoview has also been used in this setting [27]. The exam has a sensitivity of 90% for acute myocardial infarction [27]. Patients with definitely normal exams have a very low cardiac event rate both during the hospital period and during short-term follow-up, with a high negative predictive value of 99% [27]. Unfortunately, many patients do have abnormalities on their studies (such as old areas of infarction) which decreases the specificity (60%) and the positive predictive value (12%) [27]. Between 2-5% of patients with normal scans may have underlying coronary artery disease that will require revascularization and further outpatient evaluation will be required in select patients [27].
Drawbacks of imaging patients with acute chest pain are the technical and logistical difficulties of imaging patients in the acute setting, the limited availability of imaging after normal hours, and agent preparation times- Sestamibi requires 30 minutes to prepare the dose and has a shelf life of only 6 hours (which would require preparation 4 times a day to have the dose routinely available on an emergent basis). Also- some infarcts will be missed- it has been shown that at least 3-5% of the left ventricle needs to be involved to visualize an area of hypoperfusion [56,92]. Generally, missed infarcts will be small, non-Q wave inferior infarcts which will usually have an uncomplicated course [56], however, these small infarcts could be detected with troponins [92]. In fact, up to 34% of chest pain patients with normal perfusion by SPECT imaging may have an acute coronary syndrome (such as unstable angina) [92].
Imaging the Acute MI
The purpose of reperfusion therapy in patients with acute myocardial infacrtion is to achieve significant myocardial salvage and to limit the extent of irreversible tissue damage [20]. Salvaged myocardium is defined as the the difference between the initial area at risk and the final infarct size. Even a satisfactory angiographic result after PTCA does not always imply effective tissue reperfusion with consequent myocardial salvage [20]. Technetium based perfusion agents such as Sestamibi or Tetrofosmin can be injected in the emergency room to patients experiencing acute myocardial infarction. After initiation of reperfusion therapy and stabilization, images can be obtained which represent the extent of myocardium at risk at the time of infarction [50]. Subsequent images performed prior to discharge can be compared to the original exam and can assess the degree of myocardial salvage and viability [7,21].
There is excellent correlation between the size of histologic infarction and the measured region of absent perfusion on tomographic images. The absolute minimal activity (ie: the lowest pixel count) within an area of infarction, is strongly predictive of the eventual infarct size and the presence or absence of collateral flow. Although correlation with viability is reasonably high in the setting of acute infarction, cellular myocardial function does not immediately return to normal following revascularization and follow-up exams should be delayed for a period of time prior to reimaging [21]. Sestamibi uptake may not return to normal for up to 14 days following MI, reflecting metabolic derangements of tracer uptake or persistent microvascular dysfunction which limits the return of flow. The amount of salvaged myocardium is typically completely demonstrated by 7 days following revascularization on Tc-tetrofosmin imaging [21].
Another important factor in the evaluation of patients following emergent reperfusion for acute infarction is the resultant left ventricular ejection fraction (LVEF) [20]. Unfortunately, gated SPECT ejection fraction may not be accurate in the immediate post infarct period due to post-ischemic stunning and persistent contractile dysfunction [20]. The demonstration of contractile reserve within asynergic segments using dobutamine echocardiography (inotropic stimulation) can identify viable, but "stunned" myocardium [20]. The detection of any contractile reserve (even minimal wall motion) in the infarcted zone is an accurate predictor of increased LVEF during late follow-up [20].
An area of reverse-redistribution can be seen following PTCA in patients with acute MI- indicating that the ability of myocytes to retain the tracer may be impaired in stunned myocardium (possibly related to loss of the normal membrane potential or mitochrondrial injury) [84,104].
Imaging in the early post-infarct period:
In the post-infarct period, patients with evidence of ischemia on myocardial perfusion imaging have a significantly higher risk for subsequent cardiac events compared to patients without ischemia [42,67]. The greater the extent of ischemia, the more likely patients are to have a subsequent event [42,50]. Gated LVEF determination also provides prognostic information. Patients with post-infarct LVEF's less than 40% have a 3 fold increased risk for cardiac death or infarction [42]. Even with submaximal exercise, SPECT imaging is more likely to demonstrate regions of ischemia compared to ECG findings alone [50]. Pharmacologic stress imaging can also be employed as early as one to two days following acute myocardial infarction allowing very early risk stratification [50]. With pharmacologic stress, patients with small (less than 10%) or predominantly nonischemic defects can generally be treated conservatively, while patients with more extensive ischemia should be managed more aggressively due to their higher risk for subsequent cardiac event [50].
The INSPIRE trial was performed to determine risk stratification and best treatment method based upon perfusion exam findings in the early post MI period [106]. Overall, the extent of the infarct and the amount of residual ischemia were the best predictors of subsequent events [106]. Patients with small perfusion defects (less than 20% LV) were considered low risk and were targeted to receive medical therapy [106]. The subsequent rate of re-infarction/death in this group was 1.8% and coronary revascularization did not improve outcome in this group [106]. The OAT trial has also demonstrated no prognostic advantage to stenting of an occluded infarct-related artery compared to medical therapy alone in patients with minimal or no residual ischemia [106]. Patients with large (over 20%) defects and little (under 10%) ischemia were felt to be intermediate risk, but thought unlikely to benefit from coronary revascularization [106]. The cardiac event rate in this group was higher, but there was no signficant difference between medical treatment versus revascularization (13.9% versus 14.7%) [106]. Patients with large (over 20%) defects and ischemia (greater than 10%) with LVEF's under 35% were defined as high risk and encouraged to undergo revascularization [106]. This group was found to benefit the most from revascularization with a decrease in cardiac events from 32% to 10% [106]. For this same group of patients (over 20% perfusion defect and more than 10% ischemia) but preserved LV function, intensive medical therapy was as effective as coronary revascularization [106].
Patients with known or suspected CAD
Technetium agent myocardial perfusion imaging yields incremental prognostic information towards the identification of patients at risk for cardiac events [15]. Patients with adequate exercise stress and a normal perfusion exam have an overall annualized cardiac event (MI or cardiac death) rate of less than 0.5-2% per year [8,10,15,41,44]. From a multicenter registry, the annualized cardiac death rate for patients with a normal tetrofosmin exam has also been shown to be very low (0.6%) [40]. However, even if the perfusion scan is normal, it has been demonstrated that the cardiac death or non-fatal infarction rate is higher in patients with previously document coronary artery disease [44] (about 2% per year [49]). Other factors associated with a higher risk for events, despite a normal perfusion scan include pharmacologic stress, diabetes mellitus, males gender, and increasing age [44,49,52]. Thus, in specific patient populations, close follow-up may be warranted with serial testing in as early as one year [49]. Additional testing with coronary artery calcium scoring may also be beneficial in patients with intermediate clinical risk as the exam may detect preclinical CAD that would prompt risk factor modification [108].
Conversely, an abnormal perfusion exam which demonstrates a reversible defect is associated with a significantly increased risk for cardiac events [10,112 ]. An increased number of reversible defects, the presence of defects in multiple vascular territories, and the severity and extent of reversible defects are all associated with an increased risk for subsequent cardiac event [10,14,52]. The most severe reversible perfusion defect does not necessarily reflect the cardiac territory at greatest risk for subsequent infacrtion [12]. Severe stenoses are more likely to be associated with collateral circulation and infarction is more likely to complicate acute thrombosis of a mildly obstructive plaque [12]. In patients with prior MI, even the presence of fixed perfusion defects can indicate an increased risk for subsequent cardiac events- especially for patients with abnormalities in a multi-vessel distribution [62].
The results of the myocardial perfusion exam can also aid in risk stratification and provide a guide for the most effective treatment options [15]. In patients with severely abnormal scans indicating extensive ischemia, early revascularization will result in a decreased rate of cardiac death compared to a similar group of patients treated with medical therapy [15]. Patients with mildly abnormal exams have a greater risk for myocardial infarction, rather than cardiac death, and this subgroup of patients would likely benefit most from initial initial treatment [15]. Referral to catheterization and the accompanying costs may not be required if symptoms can be controlled with medical therapy [15].
In general, patients with prior MI that are more likely to have a cardiac event tend to be more symptomatic, are more frequently diabetic, and are more likely to undergo adenosine stress imaging [31]. However, cardiac event rates have also been shown to increase as a function of SPECT abnormalities [31]. Very low event rates of less than 1% are observed in patients with small MI's and no or only mild ischemia [31]. Patients with moderate or severe ischemia, and patients with large MI's had a greater likelihood of having cardiac events [31].
In patients with stable angina pectoris:
Based upon Bayesian analysis, the probability of CAD does not change significantly in patients with a high pre-test probability of CAD and negative perfusion imaging results [77]. However- it is not known if these patients remain at high risk for subsequent cardiac events [77]. In a recent study [77] the annual event rate for patients with stable angina and a normal perfusion exam was 1.2%, compared to an event rate of 3.9% if the perfusion scan was abnormal [77]. Mutli-vessel perfusion abnormalities were associated with the greatest risk for subsequent cardiac events (4.8%) [77]. Both fixed and reversible perfusion abnormalities were predictive of mortality [77]. In this study, a policy of proceeding to angiography without performing a perfusion exam would have resulted in subjecting 30% of patients to an expensive and invasive procedure, despite an expected good outcome without intervention [77]. The study concluded that SPECT imaging provides independent information for predicting outcome in patients with stable angina [77].
Following angioplasty and stent placement in patients without myocardial infarction and following coronary artery bypass grafting:
More than 1 million coronary angioplasty and stent implantation procedures are performed annually [79]. The incidence of re-stenosis following percutaneous coronary intervention (PCI) is and patients are not necessarily symptomatic [79]. SPECT imaging can aid in identifying patients at risk for a poor long term outcome [90]. Reversible perfusion defects can be found in 30-50% of patients following coronary balloon angioplasty and the finding is associated with a high risk of restensosis [28]. Restenosis is found in 52-75% of patients with reversible defects on early imaging (less than 2 months following PCI), compared to a 12-17% incidence in patients with normal scans [79]. The incidence of hard cardiac events is also higher in patients with inducible ischemic changes [90]. The overall sensitivity for detecting restenosis by SPECT ranges from 76-94% (mean 89%), and the specificity ranges from 46-84% (mean 75%) [90]. False positive exams may occur as a result of stunned vasa vasorum in the coronary artery affecting vasodilator reserve, and this can be minimized by delaying imaging at least 4 weeks following the procedure [90].
In spite of a good angiographic appearance, intravascular ultrasound has shown that some of the reversible perfusion abnormalities can be explained by an inadequate result [28]. Other etiologies which may explain reversible perfusion abnormalities in post-angioplasty patients include a transient defect in distal vessel autoregulation or a local spasm of the vessel wall at the site of dilatation [28].
Following coronary stent placement, reversible perfusion abnormalities can be found in up to 17% of patients and the finding is also associated with an increased risk for restenosis [28]. The reversible perfusion abonrmalities may be related to impairment of the microvascular response to stress, microvascular stunning due to particulate embolization associated with the procedure, unapparent angiograhpic obstruction at or adjacent to the stent (unapparent stent-edge dissection or new accumulations of focally extruded plaque) or unrecognized incomplete stent expansion [28].
Long-term adverse outcomes are increasing in the CABG population because multivessel surgery is common, requiring improved surveillance for graft patency, progression of plaque burden, and LV function [79]. In patients that have undergone revascularization with either percutaneous intervention or CABG, the presence of reversible perfusion abnormalities adds incremental prognostic information as this finding is associated with a significantly increased risk for subsequent cardiac events- even in asymptomatic patients [45,79]. A normal study in this same cohort, is associated with a very low risk for cardiac events [45].
Evaluation of Myocardial Viability
See Myocardial Viability in the Thallium section
REFERENCES:
(1) J Nucl Med 1994; Germano G, et al. A quantitative phantom analysis of artifacts due to
hepatic activity in technetium-99m myocardial perfusion SPECT studies. 35: 356-59
(2) Am J Cardiology 1990; Maddahi J, et al. Myocardial perfusion imaging with technetium-99m sestamibi SPECT in the evaluation of coronary artery disease. 66: 55E-62E
(3) Eur J Nucl Med 1988; Taillefer et al. Myocardial perfusion imaging with 99mTc-methoxy-isobutyl-isonitrile (MIBI): comparison of short and long time intervals between rest and stress injections. Preliminary results. 13: 515-522
(4) Radiol Clin North Am 1993; Borges-Neto S, Coleman RE. Radionuclide ventricular function analysis.31: 817-830
(5) J Nucl Med 1994; Kiat H, et al. Comparative feasibility of separate or simultaneous rest thallium-201/stress technetium-99m-sestamibi dual-isotope myocardial perfusion SPECT. 35: 542-48
(6) J Nucl Med 1994; Sciagra R, et al. Evaluation of coronary artery disease using technetium-99m-sestamibi first-pass and perfusion imaging with dipyridamole infusion. 35: 1254-64
(7) J Nucl Med 1992; Gibson WS, et al. Serial tomographic imaging with technetium-99m-sestamibi for the assessment of infarct-related arterial patency following reperfusion therapy. 33: 2080-85
(8) J Nucl Med 1994; Brown KA, et al. Prognostic value of normal technetium-99m-sestamibi cardiac imaging. 35: 554-57
(9) J Am Coll Cardiol 1993; Varetto T, et al. Emergency room technetium-99m sestamibi imaging to rule out acute myocardial ischemic events in patients with nondiagnostic electrocardiograms. 22: 1804-8
(10) Chest 1999; Mandalapu BP, et al. Technetium Tc 99m Sestamibi myocardial perfusion imaging. Current role for evaluation of prognosis. 115: 1684-1694
(11) J Nucl Med 2000; Walicka MA, et al. Morphological transformation of C3H 10T1/2 cells by 99mTc-Cardiolite. 41: 1545-1551
(12) J Nucl Med 2001; Candell-Riera J, et al. Relationship between the location of the most severe myocardial perfusion defects, the most severe coronary artery stenosis, and the site of subsequent myocardial infarction. 42: 558-563
(13) J Nucl Med 1995; June; p.952-55
(14) J Nucl Med 2001; Sharir T, et al. Prediction of myocardial infarction versus cardiac death by gated myocardial perfusion SPECT: Risk stratification by the amount of stress-induced ischemia and the poststress ejection fraction. 42: 831-837
(15) Ciculation 1998; Hachamovitch R, et al. Incremental prognostic value of myocardial perfusion single photon emission computed tomography for the prediction of cardiac death. Differential stratification for risk of cardiac death and myocardial infarction. 97: 535-543
(16) J Nucl Med 1993; Villanueva-Meyer J, et al. Assessment of myocardial perfusion defect size after early and delayed SPECT imaging with technetium-99m-hexakis 2-methoxyisobutyl isonitrile after stress. 34: 187-192
(17) Eur J Nucl Med 1994; Klopper RS, et al. The excretion of radiopharmaceuticals in human breast milk: Additional data and dosimetry. 21: 144-153
(18) Semin Nucl Med 1995; Newhouse HK, Wexler JP. Myocardial perfusion imaging for evaluating interventions in coronary artery disease. 25: 15-27
(19) J Nucl Med 1995; Mahmood S, et al. Combined rest thallium-201/stress technetium-99m-tetrofosmin SPECT: feasibility and diagnostic accuracy of a 90-minute protocol. 36: 932-935
(20) J Nucl Med 1995; Cuocolo A, et al. Technetium-99m-tetrofosmin regional myocardial uptake at rest: relation to severity of coronary artery stenosis in previous myocardial infarction. 36: 907-13
(21) J Nucl Med 2001; Tanaka R, Nakamura T. Time course evaluation of myocardial perfusion after reperfusion therapy by 99mTc-tetrofosmin SPECT in patients with acute myocardial infarction. 42: 1351-1358
(22) J Nucl Med 2001; Taki J, et al. 99mTc-sestamibi retention characteristics during pharmacologic hyperemia in human myocardium: comparison with coronary flow reserve measured by doppler flowire. 42: 1457-1463
(23) J Nucl Med 2001; Nakajima K, et al. Accuracy of ventricular volume and ejection fraction measured by gated myocardial SPECT: Comparison of 4 software programs. 42: 1571-1578
(24) J Nucl Med 1997; Munch G, et al. Myocardial technetium-99m-tetrofosmin and technetium-99m-sestamibi kinetics in normal subjects and patients with coronary artery disease. 38: 428-432
(25) J Nucl Med 1999; Nichols K, et al. Influence of arrhythmias on gated SPECT myocardial perfusion and function quantification. 40: 924-934
(26) J Nucl Med 2001; Sharir T, et al. Quantitative analysis of regional motion and thickening by gated myocardial perfusion SPECT: Normal heterogeneity and criteria for abnormality. 42: 1630-1638
(27) J Am Coll CArdiol 1998; Heller GV, et al. Clinical value of acute rest technetium-99m tetrofosmin tomographic myocardial perfusion imaging in patients with acute chest pain and nondiagnostic electrocardiograms. 31: 1011-17
(28) J Nucl med 2001; Rodes-Cabau J, et al. Frequency and clinical significance of myocardial ischemia detected early after coronary stent placement.
(29) J Nucl Cardiol 2001; Choy JB, Leslie WD. Clinical correlates of Tc-99m sestamibi lung uptake. 8: 639-44
(30) J Nucl Med 2002; Sciagra R, et al. Comparison of dobutamine echocardiography and 99mTc-sestamibi tomography for prediction of left ventricular outcome after acute myocardial infarction treated with successful primary coronary angioplasty. 43: 8-14
(31) J Nucl Cardiol 2002; Zellweger MJ, et al. Risk stratification in patients with remote prior myocardial infarction using rest-stress myocardial perfusion SPECT: prognostic value and impact on referral to early catheterization. 9: 23-32
(32) J Nucl Med 2002; Shirai N, et al. Incremental value of assessment of regional wall motion for detection of multivessel coronary artery disease in exercise 201Tl gated myocardial perfusion imaging. 43: 443-450
(33) Am J Cardiol 2001; Kroll D, et al. Prognostic value of stress-gated Tc-99m sestamibi SPECT after acute myocardial infarction. 87: 381-86
(34) J Nucl Med 2002; Taki J, et al. Electrocardiographic gated 99mTc-MIBI SPECT for functional assessment of patients after coronary artery bypass surgery: comparison of wall thickening and wall motion analysis. 43: 589-595
(35) J Nucl Cardiol 2002; Knott JC, et al. Impact of acute chest pain Tc-99m sestamibi myocardial perfusion imaging on clinical management. 9: 257-262
(36) J Nucl Cardiol 2002; Simones MV, et al. Prediction of left ventricular wall motion recovery after acute myocardial infarction by Tl-201 gated SPECT: incremental value of integrated contractile reserve assessment. 9: 294-303
(37) J Nucl Med 2002; Feng B, et al. Calculation of the left ventricular ejection fraction without edge detection: application to small hearts. 43: 786-794
(38) J Nucl Cardiol 2002; Vallejo E, et al. Variability of serial same-day left ventricular ejection fraction using quantitative SPECT. 9: 377-84
(39) J Nucl Cardiol 2002; Paul AK, et al. Characteristics of regional myocardial stunning after exercise in gated myocardial SPECT. 9: 388-394
(40) J Nucl Med 2003; Shaw LJ, et al. Prognostic value of normal exercise and adenosine 99mTc-tetrofosmin SPECT imaging results from the multicenter registry of 4,728 patients. 44: 134-139
(41) J Nucl Cardiol 2003; Elhendy A, et al. Long-term prognosis after a normal exercise stress Tc-99m sestamibi SPECT study. 10: 261-266
(42) J Nucl Med 2003; Spinelli L, et al. Prognostic value of combined assessment of regional left ventricular function and myocardial perfusion by dopamine and rest gated SPECT in patients with uncomplicated acute myocardial infarction. 44: 1023-1029
(43) J Nucl Cardiol 2003; Verberne HJ, et al. Stress-related variations in left ventricular function as assessed with gated myocardial perfusion SPECT. 10: 456-463
(44) J Nucl Cardiol 2003; Beller GA. Clinical value of myocardial perfusion imaging in coronary artery disease. 10: 529-542
(45) J Nucl Cardiol 2003; Elhendy A, et al. Risk stratification of patients after myocardial revascularization by stress Tc-99m tetrofosmin myocardial perfusion tomography. 10: 615-622
(46) J Nucl Cardiol 2003; Kasai T, et al. Impact of gating errors with electrocardiography gated myocardial perfusion SPECT. 10: 709-711
(47) J Nucl Cardiol 2004; Beller GA, Bergmann SR. Myocardial perfusion imaging agents: SPECT and PET. 11: 71-86
(48) J Nucl Cardiol 2004; Allman KC, Freedman SB. Emergency department assessment of patients with acute chest pain: myocardial perfusion imaging, blood tests, or both? 11: 87-89
(49) J Nucl Cardiol 2004; Shaw LJ, Iskandrian AE. Prognostic value of gated myocardial perfusion SPECT. 11: 171-185
(50) J Nucl Cardiol 2004; Mahmarian JJ, et al. Role of nuclear cardiac imaging in myocardial infarction: postinfarction risk stratification. 11: 186-209
(51) J Nucl Med 2004; Go V, et al. The diagnostic and prognostic value of ECG-gated SPECT myocardial perfusion imaging. 45: 912-921
(52) J Nucl Cardiol 2004; Travin MI, et al. The prognostic value of ECG-gated SPECT imaging in patients undergoing stress Tc-99m sestamibi myocardial perfusion imaging. 11: 253-262
(53) J Nucl Cardiol 2004; Grossman G, et al. Quantitative Tc-99m sestamibi attenuation-corrected SPECT: development and multicenter trial validation of myocardial perfusion stress gender-independent normal database in an obese population. 11: 263-272
(54) J Nucl Cardiol 2004; Heller GV, et al. Clinical value of attenuation correction in stress-only Tc-99m sestamibi SPECT imaging. 11: 273-81
(55) Radiology 2004; Borger-Neto S, et al. Outcome prediction in patients at high risk for coronary artery disease: comparison between 99mTc tetrofosmin and 99mTc setamibi. 232: 58-65
(56) J Nucl Cardiol 2004; Kontos MC, Wackers FJ. Acute rest myocardial perfusion imaging for chest pain. 11: 470-481
(57) J Nucl Med 2004; Meine TJ, et al. The additive value of combined assessment of myocardial perfusion and ventricular function studies. 45: 1721-1724
(58) J Nucl Cardiol 2004; Druz RS, et al. Postischemic stunning after adenosine vasodilator stress. 11: 534-541
(59) J Nucl Med 2004; Kasama S, et al. Dobutamine stress 99mTc-tetrofosmin quantitative gated SPECT predicts improvement of cardiac function after Carvedilol treatment in patients with dilated cardiomyopathy. 45: 1878-1884
(60) J Nucl Cardiol 2004; Lipiecki J, et al. Influence of infarct-zone viability detected by rest Tc-99m sestamibi gated SPECT on left ventricular remodeling after acute myocardial infarction treated by percutaneous transluminal coronary angioplasty in the acute phase. 11: 673-81
(61) J Nucl Cardiol 2004; Toba M, et al. Usefulness of gated myocardial perfusion SPECT imaging soon after exercise to identify postexercise stunning in patients with single-vessel coronary artery disease. 11: 697-703
(62) J Nucl Cardiol 2004; Elhendy A, et al. Prognostic value of stress Tc-99m tetrofosmin SPECT in patients with previous myocardial infarction: impact of scintigraphic extent of coronary artery disease. 11: 704-709
(63) J Nucl Med 2004; Abidov A, et al. Integration of automatically measured transient ischemic dilatation ratio into interpretation of adenosine stress myocardial perfusion SPECT for detection of severe and extensive CAD. 45: 1999-2007
(64) J Nucl Med 2005; Leslie WD, et al. Prognostic value of automated quantification of 99mTc-sestamibi myocardial perfusion imaging. 46: 204-211
(65) J Nucl Cardiol 2005; Petix NR, et al. Can the reversible regional wall motion abnormalities on stress gated Tc99m sestamibi SPEC predict a future cardiac event? 12: 20-31
(66) J Nucl Cardiol 2005; Djaballah W, et al. Gated SPECT assessment of left ventricular function is sensitive to small patient motions and to low rates of triggering errors: a comparison with equilibrium radionuclide angiography. 12: 78-85
(67) J Nucl Med 2005; Acampa W, et al. Prognostic value of myocardial ischemia in patients with uncomplicated acute myocardial infarction: direct comparison of stress echocardiography and myocardial perfusion imaging. 46: 417-423
(68) J Nucl Cardiol 2005; Thompson RC, et al. Value of attenuation correction on ECG-gated SPECT myocardial perfusion imaging related to body mass index. 12: 195-202
(69) J Nucl Med 2005; Fricke E, et al. Attenuation correction of myocardial SPECT perfusion images with low-dose CT: evaluation of the method by comparison with perfusion PET. 46: 736-744
(70) J Nucl Card 2005; Abidov A, Berman DS. Transient ischemic dilatation associate with poststress myocardial stunning of the left ventricle in vasodilator stress myocardial perfusion SPECT: true marker of severe ischemia? 12: 258-260
(71) J Nucl Med 2005; Schaefer WM, et al. Quantification of left ventricular volumes and ejection fraction from gated 99mTc-MIBI SPECT: MRI validation and comparison of Emory cardiac tool box with QGS and 4D-MSPECT. 46: 1256-1263
(72) J Nucl Med 2005; Emmett L, et al. The role of left ventricular hypertrophy and diabetes in the presence of transient ischemic dilatation of the left ventricle on myocardial perfusion SPECT images. 46: 1596-1601
(73) Radiology 2005; Utsunomiya D, et al. Object-specific attenuaiton correction at SPECT/CT in thorax: optimization of respiratory protocol for image registration. 237: 662-669
(74) J Nucl Cardiol 2005; De Winter O, et al. Incremental prognostic value of combined perfusion and function assessment during myocardial gated SPECT in patients aged 75 years or older. 12: 662-670
(75) J Nucl Cardiol 2005; Masood Y, et al. Clinical validation of SPECT attenuation-correction using x-ray computed tomography-derived attenuation maps: multicenter clinical trial with angiographic correlation. 12: 676-686
(76) J Nucl Med 2005; Heston TF, Sigg DM. Quantifying transient ischemic dilatation using gated SPECT. 46: 1990-1996
(77) J Nucl Med 2005; Elhendy A, et al. Risk stratification of patient with angina pectoris by stress 99mTc-tetrofosmin myocardial perfusion imaging. 46: 2003-2008
(78) J Nucl Cardiol 2006; Thompson RC, Cullom SJ. Issues regarding radiation dosage of cardiac nuclear and radiography procedures. 13: 19-23
(79) J Nucl Cardiol 2006; Adams GL, et al. Role of nuclear imaging after coronary revascularization. 13: 163-169
(80) J Nucl Cardiol 2004; Druz RS, et al. Postischemic stunning after adenosine vasodilator stress. 11: 534-541
(81) J Nucl Cardiol 2006; Hung GU, et al. Worsening of left ventricular ejection fraction induced by dipyridamole on Tl-201 gated myocardial perfusion imaging predicts significant coronary artery disease. 13: 225-232
(82) J Nucl Cardiol 2006; Abidov A, et al. Gated SPECT in assessment of regional and global left ventricular function: major tool of modern nuclear imaging. 13: 261-279
(83) J Nucl Cardiol 2006; Rivero A, et al. Attenuation correction reveals gender-related differences in the normal values of transient ischemic dilation index in rest-exercise stress sestamibi myocardial perfusion imaging. 13: 338-344
(84) J Nucl Cardiol 2006; Sugiura T, et al. Usefulness of Tc-99m methoxyisobutylisonitrile scintigraphy for evaluating congestive heart failure. 13: 64-68
(85) J Nucl Cardiol 2006; Boger LA, et al. Best patient preparation before and during radionuclide myocardial perfusion imaging studies. 13: 98-110
(86) J Nucl Cardiol 2006; Pham R, Bellezuoli E. Diffuse pulmonary uptake of Tc-99m sestamibi due to chemical pneumonitis. 13: 127-129
(87) J Nucl Med 2006; Goetze S, et al. Clinically significant abnormal findings on the "nondiagnostic" CT portion of low-amperage-CT attenuation-corrected myocardial perfusion SPECT/CT studies. 47: 1312-1318
(88) J Nucl Cardiol 2006; Akinboboye O, et al. Technetium tetrofosmin myocardial perfusion imaging in women. 13: 603-604
(89) J Nucl Cardiol 2006; Elhendy A, et al. Accuracy of stress Tc-99m tetrofosmin myocardial perfusion tomography for the diagnosis and localization of coronary artery disease in women. 13: 629-634
(90) J Nucl Cardiol 2006; Shaw LJ, et al. Gated myocardial perfusion single photon emission computed tomography in the clinical outcomes utilizing revascularization and aggressive drug evalation (COURAGE) trial, veterans administration cooperative study no. 424. 13: 685-698
(91) J Nucl Cardiol 2006; Higgins JP. Increased right ventricular uptake on stress SPECT myocardial perfusion images in a patient with severe coronary artery disease. 13: 725-727
(92) J Nucl Cardiol 2006; Wyrick JJ, Wei K. Cardiac imaging in the evaluation of patients presenting to the emergency department with chest pain. 13: 749-755
(93) J Nucl Cardiol 2006; Hachamovitch R, et al. Predicting therapeutic benefit from myocardial revascularization procedures: are measurements of both resting left ventricular ejection fraction and stress-induced myocardial ischemia necessary? 13: 768-778
(94) J Nucl Cardiol 2006; Travin MI. Revascularize only for ischemia, especially if left ventricular function is poor. 13: 742-746
(95) J Nucl Cardiol 2006; Verberne HJ, et al. Multicenter intercomparison assessment of consistency of left ventricular function from a gated cardiac phantom. 13: 801-810
(96) J Nucl Cardiol 2006; Ibrahim DY, et al. Optimal SPECT processing and display: making bad studies look good to get the right answer. 13: 855-866
(97) J Nucl Med 2004; Fricke H, et al. A method to remove artifacts in attenuation-corrected myocardial perfusion SPECT introduced by misalignment between emission scan and CT-derived attenuation maps. 45: 1619-1625
(98) J Nucl Cardiol 2007; Garcia EV. SPECT attenuation correction: an essential tool to realize nuclear cardiology's manifest destiny. 14: 16-24
(99) J Nucl Cardiol 2007; Dorbala S, et al. Prognostic value of SPECT myocardial perfusion imaging in patients with elevated cardiac troponin I levels and atypical clinical presentation. 14: 53-58
(100) J Nucl Cardiol 2007; Hida S, et al. Diagnostic value of left ventricular function after stress and at rest in the detection of multivessel coronary artery disease as assessed by electrocardiogram-gated SPECT. 14: 68-74
(101) Nucl Cardiol 2007; Singh B, et al. Attenuation artifact, attenuation correction, and the future of myocardial perfusion SPECT. 14: 153-164
(102) J Nucl Cardiol 2007; Burque JM, et al. Mortality risk associated with ejection fraction differs across resting nuclear perfusion findings. 14: 165-173
(103) J Nucl Cardiol 2007; Goetze S, Wahl RL. Prevalence of misregistration between SPECT and CT for attenuation-corrected myocardial perfusion SPECT. 14: 200-206
(104) J Nucl Cardiol 2007; Matsuo S, et al. A novel clinical indicator using Tc-99m sestamibi for evaluating cardiac mitochondrial function in patients with cardiomyopathies. 14: 215-20
(105) J Nucl Cardiol 2007; Mujtaba B, et al. Anaphylactic reaction to Tc-99m sestamibi (Cardiolite) during pharmacologic myocardial perfusion imaging. 14: 256-258
(106) J Nucl Cardiol 2007; Mahmarian JJ, et al. Risk statification after acute myocardial infarction: is it time to reassess? Implications from the INSPIRE trial. 14: 282-292
(107) J Nucl Cardiol 2007; Sciagra R, et al. Influence of the postexercise acquisition delay on the detection of functional abnormalities in sestamibi-gated SPECT. 14: 334-340
(108) J Nucl Med 2007; Schepis T, et al. Added value of coronary artery calcium score as an adjunct to gated SPECT for the evaluation of coronary artery disease in an intermediate-risk population. 48: 1424-1430
(109) J Nucl Cardiol 2007; Germano G, et al. Quantitation in gated perfusion SPECT imaging: the Cedars-Siani approach. 14: 433-454
(110) J Nucl Cardiol 2007; Smelley MP, et al. A hypertensive response to exercise is associated with transient ischemic dilatation on myocardial perfusion SPECT. 12: 537-543
(111) J Nuc Med 2007; Giorgetti A, et al. Feasibility and diagnostic accuracy of a gated SPECT early-imaging protocol: a multicenter study of the myoview imaging optimization group. 48: 1670-1675
(112) J Nucl Cardiol 2007; Kapetanopoulos A, et al. Regional wall-motion abnormalities on post-stress ekectrocardiographic-gated technetium-99m sestamibi single-photon emission computed tomography imaging predict cardiac events. 14: 810-817