In a recent interview, visual attention research expert Jeremy Wolfe, MD, of Harvard Medical School in Cambridge, MA, discussed an emerging trend of integrating eye gaze data from radiologists into AI algorithms.
The approach has met with early success in mammography and x-ray models, and with more development, it could help reduce perceptual errors (“misses”), as well as help solve the problem of labeling images, the research suggests. More importantly, Wolfe noted, it could make AI a more collaborative partner.
“When you're feeding the human data into the model, what you're really trying to do, I think, is to make that model in a sense more human, to make it a better partner for another human doing the task,” Wolfe said.
Wolfe, who recently penned an editorial on the subject of AI and behavioral research, is a radiologist and ophthalmologist and heads the Visual Attention Lab at Harvard. He explained that efforts to integrate eye movements of radiologists into AI aren’t about training models to identify just the troubling spots on images, but to essentially learn what’s behind the eye movements themselves.
And while training AI to learn how to scan an image in a similar way to radiologists could raise fears that AI will eventually replace radiologists, we’re not likely to reach that point, Wolfe said.
“There's way too many images out there. If the AI companion can help you with that, great. I don't think the radiologists need to worry about switching careers just yet,” he said.
AI trained on eye movements could, in fact, be a boon for the problem of labeling images.

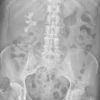


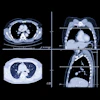
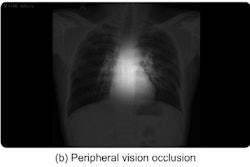









![Representative example of a 16-year-old male patient with underlying X-linked adrenoleukodystrophy. (A, B) Paired anteroposterior (AP) chest radiograph and dual-energy x-ray absorptiometry (DXA) report shows lumbar spine (L1 through L4) areal bone mineral density (BMD). The DXA report was reformatted for anonymization and improved readability. The patient had low BMD (Z score ≤ −2.0). (C) Model (chest radiography [CXR]–BMD) output shows the predicted raw BMD and Z score in comparison with the DXA reference standard, together with interpretability analyses using Shapley additive explanations (SHAP) and gradient-weighted class activation maps. The patient was classified as having low BMD, consistent with the reference standard. AM = age-matched, DEXA = dual-energy x-ray absorptiometry, RM2 = room 2, SNUH = Seoul National University Hospital, YA = young adult.](https://img.auntminnie.com/mindful/smg/workspaces/default/uploads/2026/04/ai-children-bone-density.0snnf2EJjr.jpg?auto=format%2Ccompress&fit=crop&h=112&q=70&w=112)