Newly-diagnosed prostate cancer patients who undergo PET scans versus bone scans are more than twice as likely to receive androgen receptor pathway inhibitors (ARPIs), according to a research letter published May 7 in JAMA Oncology.
The findings represent the first national-scale evidence of an association between prostate-specific membrane antigen (PSMA) PET use and differences in treatment for advanced prostate cancer, noted lead author Michael S. Leapman, MD, a urologic oncologist at Yale School of Medicine, and colleagues.
“These findings underscore patterns of clinical management associated with more sensitive cancer imaging,” the group wrote.
PSMA-PET detects regional and distant metastatic prostate cancer with significantly greater sensitivity than conventional imaging (CT or bone scan) and has been rapidly adopted since receiving national approval in 2021, the authors explained. Yet the extent to which imaging-associated stage migration is occurring or altering treatment decisions remains poorly understood, they noted.
To assess the issue, the researchers conducted a retrospective cohort study of 5,893 Blue Cross Blue Shield beneficiaries between the ages 40 to 89 who were newly diagnosed with prostate cancer between July 2021 and December 2023. Of these, 1,581 received PSMA-PET scans and 4,312 underwent bone scans. The primary outcome was initiation of ARPIs within 12 months after diagnosis. Secondary outcomes included receipt of systemic therapy, androgen deprivation therapy, chemotherapy, radiotherapy, and radical prostatectomy.
Key findings included the following:
ARPI therapy was initiated in 15.6% of PSMA-PET patients versus 7.7% of bone scan patients (p < 0.001).
In adjusted analysis, PSMA-PET was associated with 2.4-fold higher odds of ARPI initiation (OR 2.40, 95% CI 1.92–3.00).
Any systemic therapy was more common among PSMA-PET patients (50.4% versus 40.0%).
PSMA-PET patients were less likely to undergo radical prostatectomy (44.5% versus 49.6%) and more likely to receive primary radiotherapy (47.5% versus 39.5%).
Radiotherapy to secondary cancer sites was nearly three times more common in PSMA-PET patients (6.4% versus 2.4%).
PSMA-PET use surpassed bone scan in 2023, reflecting rapid national adoption.
"As PSMA-PET use grows, enhanced detection of previously occult disease stands to increase eligibility for intensified systemic therapies, with implications for cumulative toxic effects and health care value," the researchers wrote.
The authors noted limitations, including the lack of clinical data such as Gleason grade and PSA levels, absence of imaging findings distribution, and the observational design, which cannot rule out confounding from patient and clinician-level factors.
“Further studies are needed to determine whether earlier treatment based on molecular imaging is associated with improved survival and quality of life,” the group concluded.
The full study can be found here.




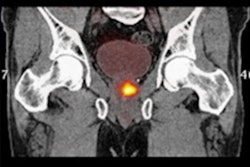




![A 53-year-old patient (patient number four) with a recurrent pituitary adenoma with extension of a cystic component of disease to the medial temporal lobe apparent on MRI (contoured in blue), and extension of disease to the left sphenoid bone and orbital apex apparent on [68Ga]Ga-DOTA-TATE (contoured in yellow).](https://img.auntminnie.com/mindful/smg/workspaces/default/uploads/2026/04/pituitary-tumor.QGsEnyB4bU.jpg?auto=format%2Ccompress&fit=crop&h=112&q=70&w=112)