Despite CT angiography (CTA) being the gold standard, Doppler ultrasound is used almost universally for monitoring liver transplant recipients, according to survey findings presented April 15 at ARRS 2026.
There is also significant variability in protocols, timing, frequency, and reporting standards for post-transplantation imaging by transplant center, said Morgan Young-Speirs, MD, from the University of British Columbia in her presentation.
“This survey confirms that imaging is widely used for post-operative monitoring of liver transplants,” she said.
Imaging plays a key role in monitoring potential complications that occur after liver transplantation. Some complications that are life- and graft-threatening include hepatic artery thrombosis, portal vein thrombosis, and hepatic vein outflow obstruction.
However, there is no established guideline or consensus regarding frequency for post-operative imaging in liver transplant patients. While some experts call for Doppler ultrasound within 24 hours followed by subsequent imaging only if concerns arise, others recommend daily Doppler ultrasound in the first post-operative week.
Young-Spiers and colleagues issued surveys to North American liver transplant centers to compare post-operative imaging practices. The study included 58 responses from 41 institutions across 25 U.S. states and Canadian provinces.
She presented the following results:
Two out of three centers reported following a formal postoperative imaging protocol.
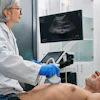
Almost all centers (98%) said Doppler ultrasound is the initial imaging modality used following liver transplantation.
Nearly half of centers (47%) said they perform the first postoperative imaging exam on post-operative day 0, with 41% saying they perform the first exam on post-operative day 1.
All respondents said that Doppler ultrasound includes assessment of hepatic artery and portal and hepatic vein patency.
Young-Speirs also noted variability in routine reporting of resistive indices, peak systolic velocity, anastomotic turbulent flow, and the presence of tardus parvus waveforms.
 A survey study presented at ARRS 2026 by Morgan Young-Speirs, MD, evaluated trends in monitoring liver transplant recipients post-operation across U.S. and Canadian transplant centers.Morgan Young-Speirs, MD
A survey study presented at ARRS 2026 by Morgan Young-Speirs, MD, evaluated trends in monitoring liver transplant recipients post-operation across U.S. and Canadian transplant centers.Morgan Young-Speirs, MD
About one in five centers (21%) said they perform follow-up imaging routinely during the initial transplant admission, while 79% said they perform more imaging exams only if clinically warranted.
And over half of centers (52%) said they image liver transplant recipients on an as-needed basis after discharge. Doppler ultrasound was the most popular modality in this area at 57%, followed by MRI at 27% and CT at 14%. Young-Speirs noted that about half of centers have a dedicated transplant radiologist interpreting images.
The results could help direct future guidelines, she said, and suggested that Doppler ultrasound’s high use among transplant centers is due to its affordability and accessibility, as well as using no radiation.
Young-Speirs also noted the fact that most centers perform initial post-operative imaging on days zero or one likely reflects concern for early vascular complications.
“Despite practice variations, there have been several studies that support using Doppler ultrasound in the first week for identifying complications and leading to improved outcomes,” she said. “But I think there’s still certainly work to be done in terms of exactly what protocol that should be.”
Young-Speirs said the next phase of the team’s study is to observe outcomes and detection rates of Doppler ultrasound for vascular complications for liver transplants that have occurred within the past three years.