Yttrium-90 radiation segmentectomy can be optimized to drive complete tumor destruction rates above 90% in liver cancer patients awaiting transplant, according to a study published May 5 in Radiology.
The finding is from an analysis of modifiable treatment parameters and outcomes after the minimally invasive procedure among 303 patients at seven liver transplant centers across the U.S., noted lead author Zachary T. Berman, MD, of the University of California, San Diego, and colleagues.
“Improvements in technique may achieve higher rates of [complete pathologic necrosis]. The procedure is associated with numerous variables, which can be adjusted to potentially optimize outcomes,” the group wrote.
Liver transplant offers the best long-term outcomes for patients with hepatocellular carcinoma (HCC) and cirrhosis, but patients often wait months for a donor organ, the authors explained. As of 2023, yttrium-90 (Y-90) radioembolization has become the most frequently used local-regional therapy in the U.S. for bridging patients with HCC to liver transplant, yet despite promising rates of complete pathologic necrosis (CPN) reported with the procedure, improvements in technique may achieve higher rates of CPN, they noted.
To that end, the group pooled data from seven liver transplant centers, analyzing 303 patients with 364 tumors treated between January 2016 and December 2024. All patients had previously-untreated HCC and underwent radiation segmentectomy using glass microspheres before transplant. The overall complete pathologic necrosis rate was 68%.
According to the analysis, the positive predictive value for CPN at the time of transplant was 91% if all of the following threshold criteria were met: microsphere specific activity of at least 1,087 Bq, perfused volume radiation absorbed dose of at least 440 Gy, angiosome-to-tumor volume ratio of at least 16, and microsphere per milliliter of at least 8,000. Meeting just one threshold predicted complete tumor destruction in 74% of cases, with the rate climbing stepwise as additional thresholds were met, the researchers reported.
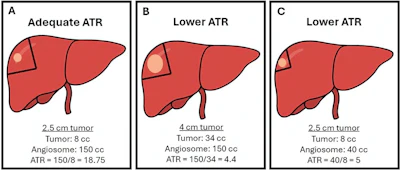 Illustrations show the role of angiosome-to-tumor volume ratio (ATR) in different clinical scenarios based on tumor and treatment angiosome volume. The pale orange oval represents the tumor within the liver, and the pie-shaped region encompassed by the black lines represents the angiosome. (A) An adequate ATR (≥16) is reached when treating tumor and an accompanying appropriate volume of expendable surrounding normal parenchyma, such as a 2.5-cm tumor within a 150-mL treatment angiosome. Lower (inadequate) ATR can occur with superselective administrations, such as (B) attempting to treat a larger (4-cm) tumor within the same 150-mL angiosome, which proves suboptimal, and (C) attempting to treat the same 2.5-cm tumor within a reduced angiosome (40 mL).RSNA
Illustrations show the role of angiosome-to-tumor volume ratio (ATR) in different clinical scenarios based on tumor and treatment angiosome volume. The pale orange oval represents the tumor within the liver, and the pie-shaped region encompassed by the black lines represents the angiosome. (A) An adequate ATR (≥16) is reached when treating tumor and an accompanying appropriate volume of expendable surrounding normal parenchyma, such as a 2.5-cm tumor within a 150-mL treatment angiosome. Lower (inadequate) ATR can occur with superselective administrations, such as (B) attempting to treat a larger (4-cm) tumor within the same 150-mL angiosome, which proves suboptimal, and (C) attempting to treat the same 2.5-cm tumor within a reduced angiosome (40 mL).RSNA
Future studies to evaluate how CPN following local therapy impacts HCC survival and to prospectively confirm optimal treatment parameters for radiation segmentectomy would further advance disease management, the researchers concluded.
In an accompanying editorial, Andrew Gordon, MD, PhD, and Robert Lewandowski, MD, both of Northwestern University in Evanston, IL, wrote that the study reflects a move from art to science.
“This work reflects intentional progress to advance Y-90 radiation segmentectomy from an art form at select specialized centers, where desirable outcomes are often routine, toward a reproducible and potentially generalizable science with specific criteria to achieve CPN at any center offering transarterial radioembolization,” they wrote.
Because CPN after local-regional therapy is linked to reduced risk of recurrence and improved survival, it follows logically that transplant centers that pursue CPN will offer their patients better outcomes, Gordon and Lewandowski wrote.
The full study is available here.