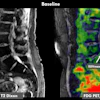
Quantitative measures obtained from the MRIs of people with scarring fibrosis conditions have been curated and analyzed to generate a new type of "fibrotic health" scoring system, according to a May 14 presentation at the ISMRM meeting in Cape Town, South Africa.
The ISMRM award-winning presentation focused on quantitative body metrics from participants with and without fibrotic conditions. Fibrotic conditions can cause significant changes to MRI-measures of the kidneys, liver, pancreas, spleen, heart, and lungs, noted the group supervised by Prof. Sue Francis, Dr. Eleanor Cox, and Prof. Dorothee Auer from the University of Nottingham in the U.K.
"Population level MRI changes in the UK Biobank allowed MRI patterns associated with fibrotic disease to be identified," wrote the group, including presenting author Margot Roeth and colleagues from the National Institute for Health Research (NIHR), Imperial College, and Guy's and St Thomas' NHS Foundation Trust.
Multimorbidity is defined as the co-occurrence of two or more chronic conditions, and the project is part of a DEMISTIFI grant, otherwise known as "Defining Mechanisms Shared Across Multiorgan Fibrotic Disease." The project's goals are to prevent the development of long-term multimorbidity.
Fibrosing patterns
To isolate fibrosing patterns, researchers worked from 60,382 abdominal and cardiac MRI image datasets and 6,540 kidney image datasets, removing certain images collected with abnormally high/low heart rate (HR)/high HR variance between scans, unphysiologically high/low organ volume, or poor organ segmentation. The study used UK Biobank data alongside local imaging data, Roeth said.
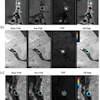
Using machine learning, the researchers estimated volume and surface area for each organ. They factored in subcutaneous and visceral adipose tissue (SAT and VAT); the liver, pancreas, spleen, kidneys, lung masks; and fat fraction, T2*, and iron for each organ. They noted that liver, pancreas, spleen, and kidney cortex and medulla (and corticomedullary difference [CMD]) ShMOLLI T1 values were computed and HR-corrected.
The researchers then classified participants in three categories that they then used to generate an MRI-based FMMS to assess risk.
Participants who were classified as "super healthy" had no fibrotic or chronic conditions. "Normal-control" participants appeared to have no fibrotic disease but possibly had chronic conditions (approximately 21,000 were in each group). Participants with a fibrotic disease were classified into one or more of 11 fibrotic (FIB) buckets defined from a Delphi study, according to the group.
Strongest patterns
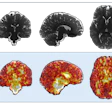
Each abdominal and cardiac MRI metric was compared to the normal control group to define significant MRI metrics related to each FIB bucket, and those with single or multiorgan (≥2) fibrosis. From these, a heatmap of Cohen’s d values was used to generate a MRI pattern for each bucket. The patterns were then correlated between buckets, and the FIB groups were tested against the normative model to generate the scores, Roeth explained.
According to the results, 9,617 participants had single fibrosis, and 2,028 had multiorgan fibrosis. Researchers observed the strongest MRI patterns in the heatmap for liver-, diabetes-, urinary-, and systemic-FIB categories.
 Margot Roeth and ISMRM
Margot Roeth and ISMRM
"Multiorgan fibrosis was linked to increased liver and pancreas T1 and reduced kidney CMD T1, increased T2* and fat in these organs, as well as increased SAT and VAT," the group noted. Comparing MRI patterns between FIB buckets showed liver-, diabetes-, biliary-, skeletal-, and intestinal/pancreatic-FIB were strongly correlated as well, they added.
"The multiorgan fibrosis MRI pattern correlated with 7 FIB buckets, suggesting different fibrotic conditions lead to similar effects on MRI-measured metrics," the group found. "The MRI-based FMMS was a sensitive measure of predicted mortality."
In addition, cardiovascular FIB strongly correlated with intestinal/pancreatic-FIB, urinary- and pulmonary-FIB; pulmonary FIB with intestinal/pancreatic- and urinary-FIB; and urinary-FIB with intestinal/pancreatic-FIB, the group observed.
The DEMISTIFI study has created a cohort of patients at risk of multimorbid fibrotic disease, who have been phenotyped for development of presymptomatic multiorgan fibrosis using genetics and imaging characteristics linked to physiology and pathobiology, according to an overview of the study.
FMMS is now being assessed in local primary disease-focused cohorts. The findings may enable early detection and aid development of therapies to treat multiorgan fibrosis, Roeth and colleagues said.
Check out AuntMinnie’s full coverage of ISMRM 2026 on our ShowCast.