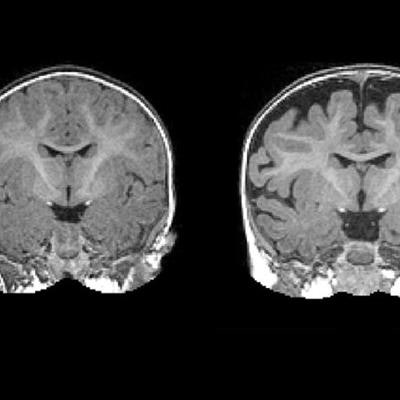
Using MR imaging, researchers have found that children diagnosed with autism at 2 years of age had a substantially greater amount of extra-axial cerebrospinal fluid (CSF) when they were 6 and 12 months old, according to a study published online March 6 in Biological Psychiatry.
Increased CSF on MRI predicted with nearly 70% accuracy which infants would eventually be diagnosed with autism, and the greater the CSF at 6 months, the more severe the autism symptoms at 2 years of age. On the positive side, the early discovery of higher CSF levels could provide pediatricians with early warning signs of autism and prompt targeted treatment.
While there's likely not one cause behind the development of autism, improper CSF flow could be one important mechanism, according to first author Mark Shen, PhD, from the University of North Carolina.
For the study, the researchers enrolled 343 infants, 221 (64%) of whom were at high risk of developing autism because an older sibling had the condition. Forty-seven infants (14%) were diagnosed with autism at 24 months; Shen and colleagues compared their MRI scans with those of other infants with no signs of autism (Biol Psychiatry, March 6, 2017).
The 6-month-old infants who eventually went on to develop autism had 18% more CSF than 6-month-olds who did not develop the condition. In addition, 6-month-old infants with CSF levels 24% greater than their counterparts went on to develop the most severe symptoms of autism. Those levels of CSF remained elevated when the subjects reached 12 and 24 months of age.
Shen and colleagues also noted that infants with greater amounts of CSF at six months often had poorer motor skills, such as head and limb control.
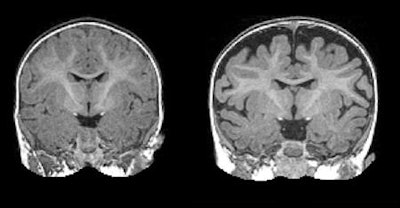 MRI of a 6-month-old baby (right) diagnosed with autism at 2 years of age. The dark space between the brain folds and skull indicates increased amounts of CSF. By comparison, a 2-year-old (left) who was not diagnosed with autism at age 2 shows less CSF. Images courtesy of the Carolina Institute for Developmental Disabilities and Biological Psychiatry.
MRI of a 6-month-old baby (right) diagnosed with autism at 2 years of age. The dark space between the brain folds and skull indicates increased amounts of CSF. By comparison, a 2-year-old (left) who was not diagnosed with autism at age 2 shows less CSF. Images courtesy of the Carolina Institute for Developmental Disabilities and Biological Psychiatry.By using the elevated CSF as a benchmark, the researchers were able to predict with approximately 70% accuracy which babies would later be diagnosed with autism. While it is not a perfect predictor of autism, the differences in CSF are observable on a standard MRI scan.
"In the future, this sort of CSF imaging could be another tool to help pediatricians detect risks for autism as early as possible," Shen said.
This paper follows a similar 2013 study in which Shen and colleagues found substantially greater volumes of CSF in babies who went on to develop autism. However, that research only included 55 babies, 10 of whom developed autism. The current study replicates and validates the previous findings within a larger cohort.


![Overview of the study design. (A) The fully automated deep learning framework was developed to estimate body composition (BC) (defined as subcutaneous adipose tissue [SAT] in liters; visceral adipose tissue [VAT] in liters; skeletal muscle [SM] in liters; SM fat fraction [SMFF] as a percentage; and intramuscular adipose tissue [IMAT] in deciliters) from MRI. The fully automated framework comprised one model (model 1) to quantify different BC measures (SAT, VAT, SM, SMFF, and IMAT) as three-dimensional (3D) measures from whole-body MRI scans. The second model (model 2) was trained to identify standardized anatomic landmarks along the craniocaudal body axis (z coordinate field), which allowed for subdividing the whole-body measures into different subregions typically examined on clinical routine MRI scans (chest, abdomen, and pelvis). (B) BC was quantified from whole-body MRI in over 66,000 individuals from two large population-based cohort studies, the UK Biobank (UKB) (36,317 individuals) and the German National Cohort (NAKO) (30,291 individuals). Bar graphs show age distribution by sex and cohort. BMI = body mass index. (C) After the performance assessment of the fully automated framework, the change in BC measures, distributions, and profiles across age decades were investigated. Age-, sex-, and height-adjusted body composition reference curves were calculated and made publicly available in a web-based z-score calculator (https://circ-ml.github.io).](https://img.auntminnie.com/mindful/smg/workspaces/default/uploads/2026/05/body-comp.XgAjTfPj1W.jpg?auto=format%2Ccompress&fit=crop&h=100&q=70&w=100)




![Overview of the study design. (A) The fully automated deep learning framework was developed to estimate body composition (BC) (defined as subcutaneous adipose tissue [SAT] in liters; visceral adipose tissue [VAT] in liters; skeletal muscle [SM] in liters; SM fat fraction [SMFF] as a percentage; and intramuscular adipose tissue [IMAT] in deciliters) from MRI. The fully automated framework comprised one model (model 1) to quantify different BC measures (SAT, VAT, SM, SMFF, and IMAT) as three-dimensional (3D) measures from whole-body MRI scans. The second model (model 2) was trained to identify standardized anatomic landmarks along the craniocaudal body axis (z coordinate field), which allowed for subdividing the whole-body measures into different subregions typically examined on clinical routine MRI scans (chest, abdomen, and pelvis). (B) BC was quantified from whole-body MRI in over 66,000 individuals from two large population-based cohort studies, the UK Biobank (UKB) (36,317 individuals) and the German National Cohort (NAKO) (30,291 individuals). Bar graphs show age distribution by sex and cohort. BMI = body mass index. (C) After the performance assessment of the fully automated framework, the change in BC measures, distributions, and profiles across age decades were investigated. Age-, sex-, and height-adjusted body composition reference curves were calculated and made publicly available in a web-based z-score calculator (https://circ-ml.github.io).](https://img.auntminnie.com/mindful/smg/workspaces/default/uploads/2026/05/body-comp.XgAjTfPj1W.jpg?auto=format%2Ccompress&fit=crop&h=112&q=70&w=112)









